Visible Clue to Health
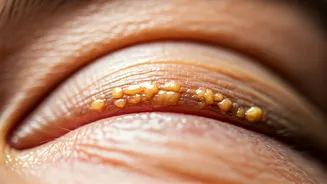
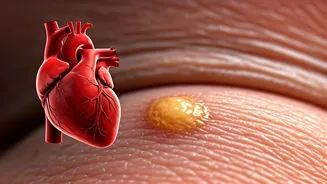
Small, yellowish deposits that emerge on or around the eyelids, particularly near the inner corners, are medically termed xanthelasma. While these are essentially
accumulations of cholesterol and fat beneath the skin, and often appear in women over 40, their significance extends far beyond a mere cosmetic concern. The eyelids, with their delicate skin and abundant blood supply, are prime locations for these lipid deposits to manifest, serving as a visible external indicator of internal metabolic processes. Therefore, what might seem like a minor skin blemish can actually be an important signal from your body about systemic cholesterol imbalances or the initial stages of atherosclerosis, a condition where plaque builds up in arteries.
Heart Attack Risk Indicator
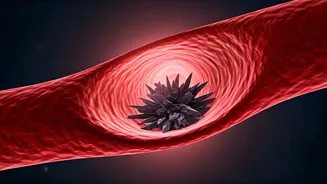
The presence of xanthelasma is notably linked to an elevated risk of heart attacks and other cardiovascular diseases. This connection becomes particularly significant when these deposits appear at an earlier age or show signs of increasing over time. Research consistently indicates that individuals experiencing xanthelasma have a considerably higher probability of developing coronary artery disease, experiencing myocardial infarctions (heart attacks), and suffering strokes, sometimes even before any typical symptoms like chest pain manifest. Cardiologists often view these eyelid deposits as an external signpost, drawing attention to potential internal vascular risks that require attention, even in the absence of immediate outward signs of distress in the cardiovascular system.
The Strength of the Link
The association between xanthelasma and heightened cardiovascular risk is not anecdotal; it is a clinically meaningful and well-documented connection. Intriguingly, this increased risk seems to persist irrespective of conventional risk factors such as age, smoking habits, or even standard cholesterol level readings. The prevailing theory suggests that xanthelasma mirrors the process of cholesterol deposition occurring within the arterial walls, much like the plaque development seen in coronary arteries. Consequently, the appearance of xanthelasma is often interpreted as an indicator of accelerated vascular aging, hinting that arterial plaque might already be developing silently within the body's circulatory system.
When Tests Appear Normal
It's important to note that xanthelasma can manifest even when routine cholesterol blood tests return normal results. This scenario doesn't necessarily negate the associated cardiovascular risk; instead, it may point to more nuanced or hidden lipid abnormalities. These could include variations in cholesterol particle size or function that aren't captured by basic tests, underlying genetic predispositions affecting lipid metabolism, diminished efficiency of HDL (high-density lipoprotein, often called 'good' cholesterol), or increased levels of inflammation and endothelial dysfunction. This underscores the critical point that consistently normal cholesterol numbers do not always equate to a low risk of cardiovascular events.
Essential Diagnostic Steps
For individuals who develop xanthelasma, a thorough cardiovascular assessment beyond standard tests is strongly recommended. This comprehensive evaluation typically involves a fasting lipid panel, alongside advanced lipid testing that might include parameters like LDL particle number, ApoB, and Lp(a). Further tests may include blood sugar and HbA1c checks to assess diabetes risk, blood pressure measurement, and high-sensitivity CRP to gauge inflammation. Depending on clinical indicators, an ECG or echocardiogram might be performed, and in select cases, a coronary artery calcium (CAC) score could be beneficial. Gathering a detailed family history also plays a crucial role, with the overarching aim being the early detection of silent atherosclerosis before a critical event like a heart attack occurs.
Removal vs. Addressing Cause
It is vital to understand that cosmetic removal of xanthelasma only addresses the visible symptom and does not rectify the underlying health issues driving their formation. The elevated cardiovascular risk persists unless the metabolic or vascular concerns are effectively managed through appropriate treatment and lifestyle modifications. Without addressing the root cause, such as persistent cholesterol abnormalities, the recurrence of xanthelasma is common. Furthermore, procedures for removal, whether topical, laser-based, or surgical, carry their own potential side effects, including changes in skin pigmentation, scarring, discomfort, and in rare instances, distortion of the eyelid. Therefore, prioritizing the management of the underlying health factors is paramount for long-term well-being.