Reassuring Findings Emerge
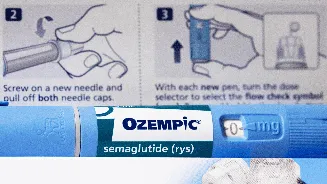
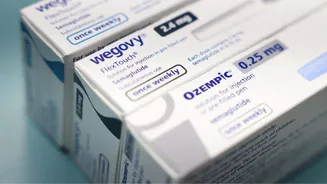
Recent extensive research, encompassing data from more than 750,000 pregnancies, is providing significant reassurance regarding the safety profile of widely-used
weight-loss medications such as semaglutide and liraglutide during pregnancy. These pharmaceutical agents, celebrated for their efficacy in managing obesity and type 2 diabetes, have understandably prompted apprehension about potential adverse effects on fetal development. Nevertheless, the outcomes derived from this large-scale investigation suggest that many of these fears might not be substantiated. The study meticulously examined a broad spectrum of potential negative impacts, including major congenital abnormalities, stillbirths, and other pregnancy-related complications. The findings indicate that infants exposed to these medications in utero did not exhibit a statistically significant increase in these adverse events when compared to a control group of pregnancies not exposed to the drugs. This evidence is particularly valuable given the escalating prescription rates of GLP-1 receptor agonists, the drug class to which semaglutide and liraglutide belong. While these medications have proven immensely beneficial for numerous individuals, their application during pregnancy has remained a subject of cautious debate due to a historical scarcity of robust real-world data.
Distinguishing Drug Usage
A critical distinction has emerged from this research concerning the rationale behind the prescription of GLP-1 receptor agonists. While these drugs are highly effective for weight management, their original development and continued use in treating type 2 diabetes present a different scenario. The study observed that when these medications were utilized for managing pre-existing diabetes, there was an associated higher risk of preterm birth. This elevated risk was notably absent when the same medications were prescribed solely for the purpose of weight loss. This critical differentiation suggests that the underlying diabetic condition itself, rather than the medication in isolation, may be a significant contributing factor to adverse obstetric outcomes like premature delivery. Specifically, women using these drugs for diabetes management showed a 70% higher risk of preterm birth with liraglutide and an 84% higher risk with semaglutide compared to those not on GLP-1 RAs. For women with pre-existing diabetes taking semaglutide, the risk of preterm birth was approximately 11%, and around 9% for liraglutide. This finding underscores the importance of considering the specific health condition being treated when evaluating drug safety during pregnancy.
Study Methodology & Implications
The research meticulously analyzed data from Danish nationwide health registries, focusing on 756,636 singleton pregnancies that concluded between October 1, 2009, and December 31, 2023. Pregnancies were categorized as inadvertently exposed if a prescription for liraglutide or semaglutide was filled within an eight-week window before or after the last menstrual period, a period encompassing early pregnancy unawareness and critical fetal development. Out of the total cohort, 529 pregnancies experienced such exposure. The researchers diligently adjusted their findings for numerous influential factors, including maternal age, body mass index (BMI), smoking habits, geographic location, educational attainment, the presence of pre-existing diabetes, and the specific month and year of pregnancy, to mitigate potential biases. These adjustments were crucial in isolating the impact of the GLP-1 RAs. The implications of these findings are substantial, suggesting that future clinical counseling for pregnant individuals inadvertently exposed to these medications should take into account the reason for their prescription. While the study provides valuable real-world evidence, it acknowledges limitations, such as the inability to definitively prove causation and the reliance on prescription redemption rather than direct evidence of drug consumption. Nonetheless, the research contributes significantly to an emerging body of evidence on the reproductive safety of GLP-1 RAs, advocating for more individualized and balanced discussions between healthcare providers and patients.