Skin's Silent Signals
Your skin can often be a mirror reflecting your internal health, and diabetes is no exception. Elevated blood sugar levels can profoundly influence your skin's
condition. This often manifests initially as minor annoyances like dry patches, persistent itching, or a rash that refuses to disappear. Many people tend to dismiss these symptoms as trivial skin reactions. However, for some, these seemingly small changes can serve as an early harbinger of diabetes. The intricate relationship between glucose regulation and skin integrity means that compromised blood flow and a weakened defense against infections, both consequences of high sugar, make the skin more vulnerable to various rashes and irritations.
Recognizing Diabetic Rashes
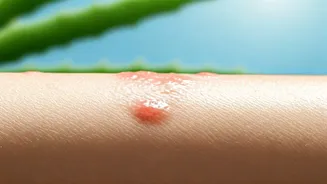
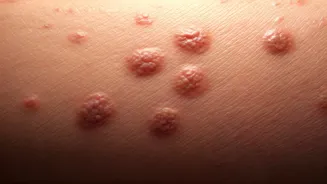
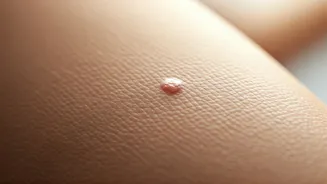
Identifying a diabetic skin rash involves noting specific characteristics that set them apart from typical skin irritations. These rashes often appear as localized areas of dryness, accompanied by redness and itching. They might also present as small, brownish spots, frequently observed on the lower limbs, arms, or the neck region. In some instances, individuals may notice a thickening or darkening of the skin, particularly in areas like the neck or underarms. The subtlety of these early indicators is crucial; persistent dryness, unexplained itching, or skin changes that heal at an unusually slow pace and do not respond to conventional topical treatments can be significant clues. Maintaining optimal blood sugar control is paramount for preserving skin health and preventing such manifestations.
Diabetic vs. Regular Rashes
Distinguishing a diabetic rash from a common allergic reaction or other regular rash is key. Unlike typical allergies, which usually arise abruptly after exposure to a specific trigger and resolve with standard treatments, diabetic rashes tend to exhibit a more chronic and recurrent nature. They often persist for extended periods, reappear frequently, and may be accompanied by other related symptoms such as pronounced dryness, susceptibility to infections, or delayed wound healing. A significant difference lies in their response to treatment; over-the-counter remedies may offer little relief, making these rashes more persistent and difficult to overlook over time. This prolonged presence and lack of swift resolution are hallmarks that differentiate them.
When to Seek Help
Deciding when to consult a healthcare professional for a skin issue is essential, especially if diabetes is a concern. Experts recommend paying close attention to the duration and intensity of any rash. A skin eruption that does not improve within a few days, begins to spread, causes significant pain, or shows any signs of infection—such as increased redness, warmth, or swelling—should prompt immediate medical evaluation. Furthermore, Dr. Bansal emphasizes that slow-healing wounds or recurrent infections should never be disregarded. Diabetes can impede the body's natural healing processes, elevating the risk of more serious complications if skin issues are left unaddressed.
Broader Skin Complications
Beyond specific rashes, diabetes can contribute to a spectrum of other skin conditions. People managing diabetes are more prone to developing fungal and bacterial infections of the skin. Diabetic dermopathy, characterized by light or dark, well-defined patches, is another common manifestation. Acanthosis nigricans, a condition leading to dark, thickened skin folds typically found in areas like the neck and armpits, is also frequently associated with diabetes. General dryness and itching remain prevalent, particularly when blood glucose levels are not optimally managed. Often, the skin is among the first indicators that something is amiss internally, making vigilance regarding persistent skin changes a valuable early detection strategy.