Understanding Cholesterol's Challenge
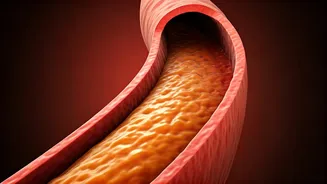
High cholesterol, particularly elevated levels of low-density lipoprotein (LDL), poses a significant risk for cardiovascular diseases worldwide. Familial
hypercholesterolemia (FH) is a common genetic disorder, affecting about 1 in 200 adults, where the body's natural system for clearing LDL from the blood is compromised. Normally, the liver uses LDL receptors (LDLR) to pull cholesterol from the bloodstream for breakdown. However, in individuals with FH, genetic defects in the LDLR gene hinder this vital cleanup process. This leads to a dangerous buildup of cholesterol over time, often without early warning signs until serious heart issues arise. Traditional treatments like statins aim to boost LDLR activity, but they prove less effective for those with severely impaired or absent receptors, prompting a search for entirely new therapeutic avenues. The focus is shifting from merely enhancing removal to exploring methods that can limit the initial production of these harmful cholesterol-carrying particles.
A New Target: ApoB
A team at the Medical University of South Carolina (MUSC) has advanced a novel strategy by targeting apolipoprotein B (apoB), a critical protein that forms the structural foundation of LDL particles. Without functional apoB, LDL particles cannot assemble correctly. This research introduces a method to reduce the overall circulation of LDL particles by interfering with their formation, irrespective of the efficiency of the LDL receptor pathway. This direct intervention at the production stage represents a significant departure from conventional cholesterol management, which primarily relies on the liver's capacity to clear existing LDL. By focusing on apoB, scientists aim to control the very genesis of LDL, potentially offering a more potent and broadly applicable solution for cholesterol regulation.
Stem Cells Power Discovery
To identify compounds capable of inhibiting apoB production, researchers employed induced pluripotent stem cells (iPSCs). These are adult cells, like skin or blood cells, reprogrammed into a stem-like state and then guided to develop into liver-like cells in a laboratory setting. This created a specialized testing environment that closely mirrors human liver function, a crucial step given the species-specific variations in cholesterol metabolism. Utilizing this human-centric platform, the team screened the South Carolina Compound Collection, a large repository of approximately 130,000 chemical compounds. This meticulous screening process led to the identification of a specific group of molecules that demonstrated a remarkable ability to significantly decrease apoB release, concurrently lowering cholesterol and triglyceride levels within the cells.
Bridging the Species Gap
Initial trials in traditional mouse models presented a hurdle, as the compounds showed limited efficacy due to differences in how mouse liver cells process cholesterol compared to human cells. To overcome this, the researchers ingeniously utilized 'Avatar' mice, which were engineered to host human liver cells. This humanized model provided a cholesterol system that closely resembled human biology, allowing for more accurate assessment of the compounds' potential. In these modified mice, the identified compounds effectively reduced lipid levels, validating their promise for human application. This step was critical in demonstrating that the discovered compounds could translate from a lab-based human cell system to a living organism with a human-like metabolic profile, strengthening the foundation for future therapeutic development.
A Path for Untreated Patients
The significance of these newly identified compounds lies in their ability to bypass the LDL receptor pathway entirely, offering a potential lifeline for patients who have few effective treatment options currently available. This groundbreaking approach, combining advanced stem cell technology with extensive compound screening, enables early-stage testing of therapies on human-like systems. This methodology reduces the dependency on less predictive animal models and is expected to increase the success rate of developing treatments that are truly effective in human patients. This innovative paradigm, where drug discovery is conducted using human systems, is heralded as the epitome of personalized medicine, paving the way for more targeted and successful interventions in managing complex health conditions like high cholesterol.