The way doctors treat diabetes and obesity is undergoing its biggest transformation in decades – and the driving force is simple: fewer injections, better results. In the latest development, the US Food
and Drug Administration approved Awiqli (insulin icodec-abae), the first and only once-weekly basal insulin for adults living with type 2 diabetes. Developed by Novo Nordisk, the approval marks a significant turning point: for the first time, a person with type 2 diabetes who needs insulin won’t have to inject themselves every single day.
The new drug reduces the burden of basal insulin administration from 365 injections a year to just 52.
“Once-weekly basal insulin represents a major advance by reducing injections from 365 to about 52 per year, thereby significantly improving compliance. It helps overcome psychological resistance and injection fatigue, and may facilitate earlier initiation of insulin, addressing therapeutic inertia. All this will lead to better sugar control and delay of complications,” Dr Anoop Misra, chairman, Fortis C-DOC Hospital for Diabetes and Allied Sciences, told News18. “Clinical trials show it to have non-inferior or slightly better HbA1c reduction compared to daily basal insulins as available in India. This approach is particularly useful for elderly patients, those with poor adherence, and individuals on multiple medications.”
Similarly, Dr Ambrish Mithal, chairman and head of endocrinology and diabetes at Max Healthcare, calls it straightforward progress for the right patients. “For people with type 2 diabetes on basal insulin, icodec can replace what they are currently taking. The efficacy is similar.”
How does it work?
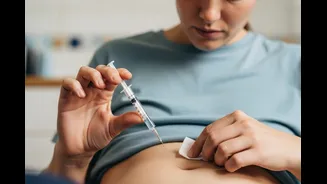
Basal insulin is the “background” insulin that keeps blood sugar stable throughout the day and night, even when you are not eating. Until now, patients had to inject it every day — for life. Awiqli is a long-acting insulin that delivers a full week’s worth of basal insulin coverage in a single shot, administered once weekly.
Across five randomised controlled trials enrolling over 3,700 participants in the ONWARDS phase 3 program, once-weekly insulin icodec demonstrated statistically significant HbA1c reduction compared to standard daily basal insulins.
One nuance doctors will watch: patients treated with Awiqli had a higher incidence of hypoglycemic events, particularly on days 2 to 4 of the dosing cycle, when insulin exposure is highest early in the week.
Mithal from Max flagged it clearly: “There may be a slight increase in hypoglycemia (low blood sugar)… it needs to be monitored. But insulin staying longer in the blood is a big relief for a large section of patients.”
For India, where millions of diabetics avoid or delay insulin out of fear, the implications are significant. “This will be important for India, where fear of insulin injection is widespread. However, cost may be a concern,” added Misra.
Novo Nordisk expects to launch Awiqli in the United States in the second half of 2026. India’s own regulatory timeline is yet to be announced.
The next frontier: Once-a-month weight loss shots
If weekly insulin is a leap forward for diabetes, the weight loss drug pipeline is preparing an even bolder jump — monthly injections that could replace the current weekly GLP-1 shots like Ozempic and Wegovy.
Mithal lays out what’s coming. “The future is very interesting. Leading candidates include Maridebart cafraglutide (MariTide) by Amgen and Pfizer’s PF-08653944, which have demonstrated significant, sustained weight loss in studies showing up to 17–20 per cent weight loss. These are even more convenient for people to use,” he says.
These are two experimental once-monthly weight loss injections currently in clinical trials. MariTide (by Amgen) is a monthly shot that combines two hormone pathways — it activates GLP-1 receptors and blocks GIP receptors — while Pfizer’s PF-08653944 is an ultra-long-acting GLP-1 drug designed to deliver a full month’s worth of appetite and weight control in a single injection.
Dr Vinus Taneja, consultant in internal Medicine at Sir Ganga Ram Hospital, explained on the science behind these agents. The drug being furthest along is Pfizer’s PF-08653944, currently in a Phase 2b trial called VESPER-3. The data suggest that monthly GLP-1 drugs can sustain robust weight reduction after a brief initial weekly titration phase — reducing injection frequency fourfold while preserving clinical benefit.
Current weekly GLP-1 injections like semaglutide (Wegovy or Ozempic) were already a vast improvement over earlier, daily diabetes injections. But monthly is another leap — and adherence is everything in chronic disease management. “Patients who can’t keep up with a weekly schedule are less likely to stay on therapy, regain weight, and return to elevated health risk. Monthly dosing addresses that directly.”
More potent drugs in pipeline
Monthly shots are not the only development. Mithal points to a third wave of options that could arrive even sooner.
“One is more potent drugs like retatrutide, which shows greater weight loss than Mounjaro, 25 per cent or greater weight loss. Trials are already complete… It could come next year, not very far,” he said. Retatrutide is a triple agonist, meaning it activates three different hormone pathways simultaneously, producing substantially more weight loss than current dual-agonist drugs.
Oral options in the weight loss category are also advancing. “Development of oral GLP-1 drugs like orforglipron is going to increase oral options. Weight loss to the tune of 10–12 per cent — not comparable to Mounjaro or retatrutide — but it gives an easier oral option,” Mithal added. For patients who are needle-averse, this could be a game-changer.
Taneja notes that beyond weight loss, the next-generation agents are showing benefits across a cluster of related conditions — from fatty liver disease (MASH) and obstructive sleep apnea to early kidney disease. Dual and triple agonist drugs that simultaneously lower weight, blood pressure, triglycerides, and kidney inflammation may become the go-to therapy across the entire cardiometabolic spectrum.
The big picture
Taken together, these developments signal something larger than incremental drug development – daily pills, daily injections, daily reminders – is quietly giving way to a once-a-week or once-a-month paradigm.
For a country like India, carrying the world’s largest diabetes burden and a growing obesity epidemic, the shift matters enormously. Simpler regimens mean better adherence, earlier intervention, and fewer long-term complications – provided access and cost are addressed in parallel.