Recent updates from the American College of Cardiology (ACC) and the American Heart Association (AHA) have not only redefined the timeline for heart disease prevention but also shifted the core philosophy
from a 10-year risk model (what may happen in the next decade) to a lifetime risk approach (what may happen over the next 30+ years).
Dr M. Sudhakar Rao, Consultant, Cardiology, Manipal Hospital, Sarjapur Road shares all you need to know:
New Guidelines Suggest Earlier Screening, The Earlier, the Better
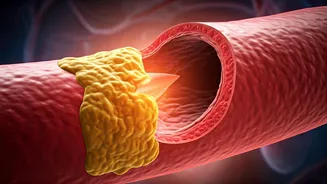
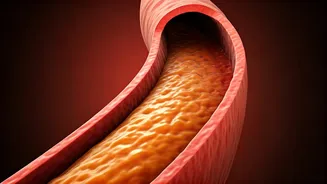
The new guidelines are based on the understanding that plaque build-up (atherosclerosis) can begin early in life.
Universal Screening: It is now recommended that all children be screened for cholesterol between the ages of 9 and 11.
Lower Age Threshold: Adults are now encouraged to undergo detailed risk assessments starting at age 30, compared to the earlier benchmark of 40.
New Tools: The PREVENT Calculator
Traditional tools like the ASCVD risk score and the Framingham score are being supplemented by a newer model PREVENT (Predicting Risk of Cardiovascular Disease Events).
Advantages
Long-term view: It assesses both 10-year and 30-year cardiovascular risk.
Broader health markers: It includes parameters such as kidney function (eGFR) and blood sugar levels (HbA1c), recognising that heart health is closely linked to overall metabolic health.
Lower Targets and New Biomarkers
“Lower is better”: LDL (“bad” cholesterol) targets have become more stringent. For high-risk individuals, the goal is now below 55 mg/dL, compared to 70 mg/dL earlier.
Lp(a) testing: A one-time lifetime test for Lipoprotein(a), a genetic marker for heart disease that is not influenced by diet or exercise is now strongly recommended for all adults.
Will These Guidelines Change Long-Term Management?
By lowering the age and risk thresholds for treatment, eligibility for statin therapy may increase, potentially starting a decade earlier than before. This raises concerns about longer durations of medication use.
While statins are generally safe, they may cause side effects such as muscle pain, slight increases in blood sugar, and, in rare cases, changes in liver enzymes.
This shift may gradually move the approach from a “lifestyle-first” strategy to an “early pill” approach, potentially creating a “patient identity” even in otherwise healthy individuals.