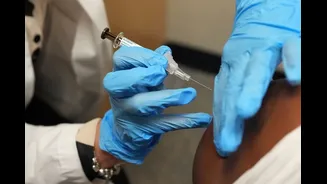
The Centre’s decision to confine the first phase of its nationwide Human Papillomavirus vaccination campaign to girls who have completed 14 years but are below 15, has triggered questions over whether
the sharply defined age cutoff is primarily guided by scientific evidence or shaped by logistical considerations.
While earlier announcements had indicated HPV vaccination for girls aged nine to 14 to prevent cervical cancer – one of the leading cancers among Indian women – the operational rollout has narrowed the focus to a single cohort.
Scientifically, Human Papillomavirus (HPV) is a common viral infection transmitted through sexual contact and is responsible for the majority of cervical cancer cases. Experts told News18 that medical evidence shows the vaccine works best when administered before exposure to the virus.
Although younger adolescents generate a stronger immune response, experts said vaccinating at 14 to 15 years old still falls well within the protective “pre-exposure” window for most girls. The age also aligns with the global goal of vaccinating girls “before their 15th birthday” under the World Health Organization’s cervical cancer elimination strategy.
There are programmatic advantages as well. Targeting 14-year-olds allows the government to focus on a clearly identifiable school-based cohort, improving coverage tracking and mobilisation. It also enables adoption of a single-dose schedule – a strategy backed by emerging global evidence – making large-scale rollout more feasible in the context of supply and funding constraints.
‘A MIX OF SCIENCE AND LOGISTICS’
Dr Neha Kumar, senior consultant, gynaecological oncology at Amrita Hospital, Faridabad, said the decision reflects calibrated thinking rather than compromise.
“I perceive the 14-15 focus as pragmatic rather than arbitrary: it aligns with the global goal of vaccinating girls by their 15th birthday and with school-based delivery/logistics aimed at older cohorts who may have missed earlier rounds,” Dr Kumar said.
She said while earlier vaccination produces a stronger immune response, the current age band remains scientifically valid.
“Younger adolescents (9-14) have a stronger immune response, which is why vaccination is better done earlier. However, 14-15 is still in the ‘pre-exposure’ window for most groups, so it is still very protective if given before sexual debut,” she said.
On the scientific basis for a single-dose approach, she said: “The KEN-SHE and DoRIS findings and pooled analyses show that a single dose offers significant protection against persistent oncogenic HPV infection. This makes a single-dose policy appealing for catch-up campaigns.”
“The World Health Organization now supports a one- or two-dose schedule for nine to 20-year-olds. This gives programmes the freedom to use a single dose for 14- to 15-year-olds when supply and coverage concerns make it the best choice. However, girls with weak immune systems still need multi-dose schedules,” she added.
Summing up the rationale, she said: “To sum up, picking 14-15 is a mix of science (it’s still within an effective immunological window) and logistics (the programme’s reach and the global 15-year target).”
Pragya Shukla, head of department, clinical oncology at Delhi State Cancer Institute believes the central objective remains vaccination before exposure.
“The best age for immunisation is before the onset of sexual activity,” Dr Shukla said. “In Indian culture it can be safely assumed that since the legal marriageable age is 18 for girls and our culture premarital sex is uncommon. This is the reason for choosing this age.”
On single-dose effectiveness, she said: “WHO and other health bodies have reviewed data that suggest single-dose effectiveness is promising.”
‘CRITICAL PREVENTION PUSH’
Even as the narrowed age band prompts discussion, oncologists have broadly welcomed the nationwide free HPV vaccination programme as a major preventive health intervention.
Dr Indu Bansal Aggarwal, group director and HOD – radiation oncology at Paras Health, Gurugram, described it as a “giant leap towards a cancer-free tomorrow”, saying it empowers young girls to take control of their health and future while protecting families from the devastating impact of cervical cancer.
Dr Agarwal stressed that vaccination must be accompanied by education on safe sexual practices and regular, age-appropriate Pap smear screening.
Similarly, Dr Dinesh Pendharkar, director of oncology at Sarvodaya Hospitals, said as an oncologist, he has seen many women present with advanced cervical cancer despite it being largely preventable. He described the nationwide free HPV vaccination programme as a powerful and practical move toward prevention, ensuring equitable access and bringing India closer to eliminating cervical cancer.
Dr Avanish Saklani, director of surgical oncology, Fortis Hospital Mulund in Mumbai, said administering the HPV vaccine at an earlier age, ideally between nine to 12 years, is known to generate a stronger immune response. However, setting a cutoff at 14 years old is a practical and scientifically sound approach.
“At this age, girls still mount a robust immunogenic response, making a single-dose strategy both effective and feasible,” Dr Saklani said.
From a safety and efficacy standpoint, multiple international trials, including those conducted in Kenya and Costa Rica, have demonstrated that a single dose provides adequate protection in younger age groups. Several countries, such as the UK’s NHS, have already adopted a single-dose schedule for average-risk adolescent girls.
“While in an ideal scenario we would expand the programme further to include younger boys and widen the eligible age group, given our large population and the significant burden of cervical cancer, this is a pragmatic and highly welcome step by the government,” he said.