The Mysterious Lp(a)
Lipoprotein(a), or Lp(a), represents a unique form of cholesterol that significantly elevates the risk of experiencing heart attacks and strokes. It's
distinct from the commonly discussed LDL ('bad') and HDL ('good') cholesterol. Lp(a) comprises an LDL-like particle bonded to a specialized protein called apolipoprotein(a). This apolipoprotein(a) component is the defining feature, bestowing upon Lp(a) its propensity to foster atherosclerosis, the insidious buildup of plaque within arterial walls. Elevated Lp(a) levels are particularly concerning when combined with other common cardiovascular risk factors like hypertension, diabetes, smoking, and obesity. It's estimated that roughly 20% of the general population carries higher-than-normal Lp(a) levels. A critical aspect of Lp(a) is that its concentration in the blood is primarily dictated by genetics, making it largely unresponsive to typical dietary adjustments or exercise regimens.
Why Lp(a) Matters
The significance of Lp(a) lies in its potent contribution to cardiovascular disease. Individuals with elevated Lp(a) face approximately a double risk of heart attack and stroke, even when their LDL cholesterol is within normal ranges. This risk is often inherited; a family history of early-onset heart disease can be a strong indicator of potentially high Lp(a) levels. Compounding the issue, current medical interventions have limited direct efficacy in lowering Lp(a). While managing other cardiovascular risk factors such as blood pressure, cholesterol, and diabetes remains vital, they don't directly target Lp(a). Therefore, early detection through a simple blood test is paramount. Screening is particularly recommended for those with a familial predisposition to premature cardiovascular disease or individuals presenting with multiple established risk factors.
How Lp(a) Harms
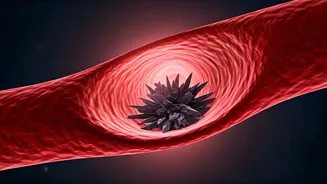
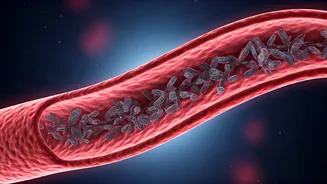
Lp(a) exacerbates heart disease risks through several detrimental mechanisms. Firstly, much like LDL, it transports cholesterol that infiltrates artery walls, leading to the gradual formation of fatty deposits, or plaques. These plaques progressively narrow the arteries, impeding blood flow and increasing the likelihood of chest pain, heart attacks, and other cardiac complications. Secondly, the apolipoprotein(a) component imbues Lp(a) with an unusual stickiness and pro-inflammatory nature. This promotes irritation within the delicate lining of blood vessels, thereby accelerating plaque development. Plaques influenced by Lp(a) are also inherently more prone to rupture, a sudden event that can precipitate acute cardiac episodes. Thirdly, Lp(a) interferes with the body's natural processes for breaking down blood clots, making clot formation more likely and persistent, which further elevates the risk of heart attack and stroke. These combined effects underscore why Lp(a) poses a threat even to individuals who otherwise appear remarkably healthy.
Targeting Elevated Lp(a)
While direct lifestyle interventions for Lp(a) are ineffective, aggressive management of other modifiable cardiovascular risk factors is essential. This encompasses maintaining a heart-healthy diet, engaging in regular physical activity, abstaining from smoking, and diligently controlling blood pressure and diabetes. Some medications commonly used to lower LDL cholesterol, such as statins, might offer a marginal reduction in Lp(a) levels, but this is not their primary therapeutic effect and may even slightly increase Lp(a) by 10-20%. However, the overall heart-protective benefits of statins generally outweigh this effect. For individuals with very high Lp(a) levels, cardiologists may implement more aggressive LDL reduction strategies, potentially combining low-dose statins with PCSK9 inhibitors, which are potent injectables that can significantly lower LDL and offer a moderate reduction in Lp(a). Promisingly, an oral daily pill is currently undergoing trials and has demonstrated substantial Lp(a) reduction, with potential availability by late 2026 or early 2027. Until then, stringent control of all other cardiovascular risk factors remains the cornerstone of prevention.
Who Needs Testing?
Given that Lp(a) levels are genetically determined and remain relatively stable throughout life, a single blood test is typically sufficient for assessment, making repeat testing generally unnecessary. The affordability of the test further encourages screening. Testing becomes particularly pertinent for individuals with a family history of heart disease, especially if it occurred at a young age. It is also recommended for those who have developed heart disease despite maintaining normal cholesterol levels, individuals with exceptionally high LDL cholesterol, or those suspected of having familial hypercholesterolemia. Furthermore, people experiencing recurrent cardiovascular events despite receiving treatment should consider an Lp(a) evaluation. A 48-year-old individual, despite being a fitness enthusiast with excellent weight, resting heart rate (48 bpm), and healthy eating habits, discovered plaque in his arteries via a calcium score test (30, with <10 considered safe) and subsequently found high Lp(a) levels (70 mg/dL, with <30 mg/dL normal), highlighting the silent risk.