Unlocking Metformin's Brain Action
Metformin, a cornerstone in diabetes management for over six decades, has primarily been understood to exert its blood sugar-lowering effects through actions
in the liver and the digestive system. However, recent scientific inquiry has unveiled a fascinating new dimension to its mechanism of action, suggesting a significant role for the brain in its efficacy. This investigation delves into how the brain, a known master regulator of overall glucose metabolism, actively contributes to metformin's therapeutic outcomes. The study challenges the long-held assumption that diabetes medications generally do not interact with the central nervous system, proposing that metformin has been subtly influencing brain pathways all along, a revelation that could revolutionize future diabetes treatment strategies by allowing for highly targeted interventions directly within the brain.
The Rap1 Protein Pathway
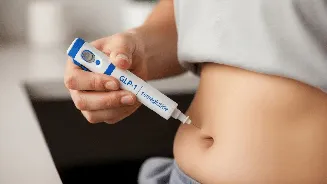
The research specifically zeroes in on a protein known as Rap1, found within a critical brain region called the ventromedial hypothalamus (VMH). This area of the brain is central to controlling feelings of fullness and sensing glucose levels throughout the body. By investigating the role of Rap1, scientists discovered that diminishing its activity within the VMH significantly enhanced metformin's ability to reduce elevated blood sugar. To validate this finding, the researchers conducted experiments using genetically modified mice that lacked Rap1 specifically in the VMH. When these mice, who were fed a high-fat diet to mimic type 2 diabetes, were administered low doses of metformin, their blood glucose levels showed no improvement. This contrasted sharply with other diabetes treatments like insulin and GLP-1 agonists, which remained effective, highlighting the indispensable role of Rap1 in metformin's brain-mediated glucose control.
Direct Brain Delivery
Further experiments provided compelling evidence for metformin's direct impact on the brain. When the diabetic mice were given metformin directly into their brains, even at doses thousands of times smaller than what is typically taken orally, a substantial decrease in blood sugar levels was observed. This remarkable sensitivity underscores the brain's potent response to the drug. The study also aimed to identify the specific types of brain cells within the VMH that are involved in relaying metformin's effects. It was observed that SF1 neurons, a particular class of nerve cells, become active when metformin is introduced into the brain, indicating their direct involvement in the drug's mechanism. Analyzing brain tissue, researchers measured the electrical activity of these SF1 neurons and found that metformin increased this activity, but crucially, only when Rap1 was present. In mice genetically engineered to be deficient in Rap1 within SF1 neurons, metformin had no discernible effect on blood sugar, definitively proving that Rap1 is a prerequisite for metformin to engage these brain cells and regulate glucose.
Reimagining Metformin's Reach
This pivotal discovery fundamentally shifts our understanding of how metformin operates. It's no longer solely viewed as a drug acting on the liver or the intestines; its influence on the brain is now undeniable. The research highlights a significant difference in the drug's required concentrations for efficacy: while the liver and digestive tract necessitate higher doses of metformin to respond, the brain reacts profoundly even to minuscule amounts. This nuanced understanding opens up exciting possibilities for developing next-generation diabetes therapies that can precisely target this newly identified brain pathway, potentially leading to more effective and individualized treatment plans for individuals living with diabetes, with fewer side effects.