The Deceptive Nature of Chest Congestion
Chest congestion, a common condition characterized by mucus buildup in the airways, can stem from various infections like colds, flu, or pneumonia. While
often presenting with mild symptoms such as a cough, it can become significantly more serious, especially in older adults. The accumulation of mucus can obstruct breathing, creating an environment ripe for secondary infections. In vulnerable individuals, this seemingly manageable ailment can act as a gateway to more profound health crises. The initial signs might be subtle, making early recognition and prompt medical evaluation paramount to prevent further complications and potential escalation into life-threatening scenarios. It's crucial to understand that what appears as a simple cough or chest discomfort could, in fact, be the nascent stage of a more severe underlying issue demanding immediate medical attention.
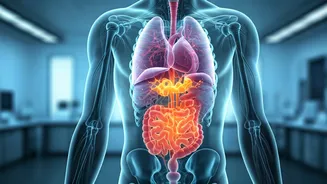
Multi-Organ Failure Explained
Multi-organ failure, also known as Multiple Organ Dysfunction Syndrome (MODS), represents a grave medical state where two or more vital organs cease to function effectively. This catastrophic cascade is often triggered by severe infections, trauma, or pre-existing chronic conditions that compromise the body's ability to respond to stress. In the context of an initial infection, such as chest congestion, the body's inflammatory response can become dysregulated, leading to a systemic breakdown. Organs like the lungs, heart, kidneys, and liver can be simultaneously affected, each failing due to lack of oxygen, impaired blood flow, or direct damage from toxins and inflammation. The interconnectedness of bodily systems means that the failure of one organ places immense strain on others, creating a dangerous feedback loop from which recovery is challenging and often requires intensive medical support.
Elderly Vulnerabilities Unveiled
Octogenarians and other elderly individuals face heightened risks when it comes to infections and subsequent complications. Their physiological reserve is often diminished due to age-related decline in immune function, reduced organ efficiency, and the common presence of comorbidities such as diabetes, hypertension, and heart disease. These underlying conditions already compromise organ systems, making them less resilient to the stress of an infection. Furthermore, the elderly may not exhibit classic infection symptoms; subtle changes like confusion, reduced appetite, or unusual fatigue can be mistaken for normal aging. This delay in recognizing and addressing an infection is critical, allowing it to progress unchecked. The cough reflex, essential for clearing the lungs, also weakens with age, leading to mucus accumulation and an increased likelihood of developing pneumonia and other respiratory infections that can rapidly spread.
The Cascade of Complications
Once an infection gains a foothold in an elderly individual, it can swiftly trigger a chain reaction leading to multi-organ failure. For instance, a lung infection can lead to Acute Respiratory Distress Syndrome (ARDS), severely impairing oxygen supply to the blood. This hypoxia then affects all organs, potentially leading to kidney injury, cardiac dysfunction, and even neurological issues like stroke. The body's response to widespread infection, known as sepsis, further exacerbates the problem by causing systemic inflammation and widespread tissue damage. Even infections originating outside the chest, like a urinary tract infection, can become life-threatening in individuals with compromised health due to diabetes or other chronic illnesses, spreading through the bloodstream and leading to septic shock and organ failure. The reduced physiological reserve means these individuals have a significantly narrower window for effective treatment.
Crucial Role of Early Intervention
The single most vital factor in averting multi-organ failure, especially in the elderly, is timely medical intervention. The challenge lies in the often subtle and easily misinterpreted initial symptoms. Caregivers and family members must be vigilant for any deviation from normal health, such as subtle changes in appetite, increased fatigue, mild confusion, or slight breathing difficulties, recognizing these as potential red flags rather than simply signs of aging. Prompt medical evaluation allows for early diagnosis and treatment, preventing infections from escalating to a critical stage. Modern medical science offers advanced life support systems in intensive care units, but the prognosis for multi-organ failure remains challenging and depends heavily on the patient's overall health, the extent of organ damage, and the speed of treatment initiation. Preventive measures, including maintaining good hydration, nutrition, and managing chronic conditions, are also fundamental in reducing the overall risk.
Environmental and Lifestyle Factors
Beyond direct medical conditions, environmental and lifestyle factors play a significant role in exacerbating the vulnerability of the elderly to severe infections. Poor air quality, particularly prevalent in urban areas, can compromise lung capacity and defense mechanisms, making individuals more susceptible to respiratory infections and hindering recovery. During periods of extreme weather, such as heatwaves, dehydration becomes a major concern, further impacting circulation and organ function, and increasing the risk of infections. Contaminated food and water can also lead to gastrointestinal illnesses that can quickly become serious in older adults. Therefore, maintaining good hygiene, ensuring safe food and water consumption, and taking precautions against environmental pollutants, like wearing N95 masks in high-pollution zones, are essential preventive strategies. Regular exercise in a clean environment also contributes to overall health and resilience.