The Nighttime Tingle
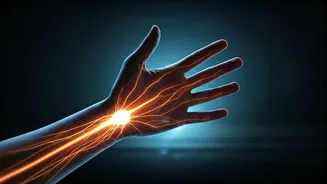
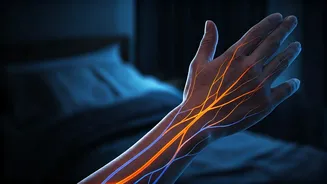
Many people experience a peculiar sensation of tingling, numbness, or even a burning feeling in their hands exclusively during the quiet of the night.
Often dismissed as a minor inconvenience, this nocturnal discomfort is frequently a significant indicator of underlying nerve stress or potential damage. Neurological experts emphasize that such recurring sensations, especially those that disrupt sleep or follow a predictable pattern, should not be overlooked. The body's physiological shifts during rest, such as altered blood flow, muscle relaxation, and changes in posture, can exacerbate existing nerve compression. For instance, the common habit of bending wrists inward during sleep can put increased pressure on the median nerve in the carpal tunnel, leading to the familiar pins-and-needles feeling. Furthermore, while movement during the day can mask subtle nerve signals, the stillness of the night amplifies them, making them more noticeable.
Doctors' Perspective
Medical professionals view nighttime hand tingling not as a diagnosis itself, but as a crucial message from the body that warrants further investigation. By analyzing the specific patterns, locations, and frequency of these sensations, doctors can begin to unravel the root cause. Carpal tunnel syndrome is a frequent culprit, characterized by pressure on the median nerve that typically affects the thumb, index, and middle fingers, and is often exacerbated by sleeping positions. However, the origin of nerve compression can also be higher up, stemming from issues within the cervical spine (neck). Beyond direct compression, systemic conditions can also manifest as peripheral neuropathy, initiating with tingling in the extremities, particularly when at rest. Conditions such as diabetes, deficiencies in vitamin B12, or thyroid imbalances are commonly associated with this type of nerve damage, highlighting that the source of the symptom can range from localized strain to broader metabolic disturbances.
When to Worry
While an occasional bout of tingling after an awkward sleep position is generally not cause for alarm, a pattern of recurrence and specific accompanying symptoms should raise concern. Medical professionals consider symptoms serious when tingling is accompanied by a noticeable reduction in grip strength, generalized hand weakness, persistent burning sensations, or an increased tendency to drop objects. These additional signs suggest that the nerves are under sustained and significant stress, necessitating prompt medical attention. The frequency of the episodes, the consistency in the affected fingers, and any gradual worsening of the sensation all contribute to identifying a problematic pattern. In medicine, consistent patterns are key indicators that a condition requires evaluation and management.
Ignoring the Signals
Nerves possess a degree of resilience, but they are not impervious to prolonged stress or damage. Initially, tingling episodes may be transient, but as pressure or damage continues, the sensation can evolve into persistent numbness. This can lead to a diminished grip strength and difficulty with fine motor skills, such as fastening buttons. In more advanced stages, the lack of adequate nerve signals can result in muscle atrophy. Early diagnosis is paramount; in many instances, symptoms can be effectively reversed with timely and appropriate interventions. However, neglecting these early warning signs can result in progressive, and potentially irreversible, nerve damage that becomes considerably more challenging to treat over time. The decision to address these symptoms early can significantly influence the outcome and the ease of recovery.
Effective Solutions
The most effective remedies for nighttime hand tingling are contingent upon identifying and addressing the underlying cause. Simple adjustments, such as improving sleeping posture, can often alleviate pressure on nerves. The use of wrist splints during sleep can help maintain a neutral wrist position, thereby reducing compression. If a deficiency is identified, such as low vitamin B12 levels, correcting this through supplements or dietary changes can provide relief. For individuals managing diabetes, maintaining stable blood sugar levels is crucial for preventing nerve damage progression. In persistent cases, doctors may recommend nerve conduction studies, diagnostic tests that measure the speed and efficiency of nerve signal transmission to precisely pinpoint the source of the problem. The foundational step, however, remains recognizing the pattern early and seeking professional medical advice.