The Brain-Skin Connection
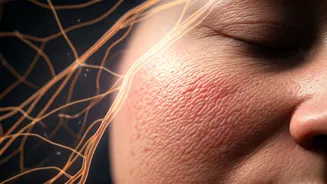
Your skin is far more than a simple outer covering; it's an active organ with its own immune system and a direct communication pathway to your brain, known
as the brain-skin axis. When you experience stress, your body releases cortisol, a hormone that can significantly disrupt the skin's normal functions. At elevated levels, cortisol impairs the skin's natural defenses, making it more permeable and susceptible to irritants. Consequently, the skin's ability to repair itself diminishes, leading to a slower healing process. This delicate interplay explains why stressful periods, whether from academic pressure, demanding work, or personal turmoil, often manifest visibly on your skin, making existing conditions worse and delaying recovery.
Cortisol's Oily Impact
One of the most notable effects of heightened cortisol levels is an increase in oil production by the skin. This surge in sebum can be particularly problematic for individuals already prone to acne. Instead of just triggering new breakouts, stress-induced oiliness exacerbates existing acne, making it more persistent and challenging to treat. The inflammatory response, coupled with increased oil, creates a perfect storm for persistent blemishes and can significantly hinder the resolution of current outbreaks, prolonging the discomfort and visual impact of acne.
Overlooked Early Signals
Many people dismiss the initial signs that their skin is under stress, often attributing them to external factors like weather changes or the use of new skincare products. These subtle indicators include a loss of radiance, making the skin appear dull and lackluster despite adequate sleep. You might also notice dry patches on areas of your face or body that are typically well-hydrated, or a heightened sensitivity where products that were once tolerated now cause irritation. Itchiness without an apparent cause is another common, yet frequently ignored, symptom. These are not random occurrences but rather the skin's first alarm bells, signaling an internal reaction to stress that began weeks prior.
Conditions Tied to Stress
A significant body of medical research firmly establishes a link between mental stress and a range of dermatological conditions. These include, but are not limited to, acne, psoriasis, eczema, rosacea, and seborrheic dermatitis. The physiological changes triggered by stress can directly contribute to the onset or exacerbation of these issues. For instance, in cases of psoriasis, flare-ups have been observed to correlate precisely with stressful life events, making the skin almost a chronicle of emotional turmoil. Furthermore, stress demonstrably slows down the skin's natural healing processes. Small wounds, post-inflammatory hyperpigmentation from acne, and other marks take considerably longer to fade when the body is under prolonged stress, which can lead to frustration and a feeling of helplessness.
Treatment Beyond Skin
Addressing skin problems solely through topical treatments or standard dermatological interventions may not be sufficient if the underlying cause is stress. For individuals experiencing persistent or recurring skin issues that resist conventional care, a deeper investigation into their life circumstances is often necessary. As one dermatologist noted, the skin often reveals truths that patients may not consciously acknowledge; it can display signs of stress long before the individual feels its full impact internally. Therefore, stress management is not merely a supplementary recommendation but can be the critical missing element in a comprehensive treatment plan for many skin conditions.