Visible Clues Explored
While outward signs like skin tags around the neck and a widening waistline might feel like definitive indicators of insulin resistance, it's crucial to understand
their limitations. These physical changes, particularly abdominal fat accumulation, can indeed be early whispers of the body's struggle with insulin. Chronically elevated insulin levels may encourage skin cell proliferation, leading to the development of those small skin growths. Similarly, central obesity is often linked to metabolic disturbances. However, relying solely on these visible cues for self-diagnosis is ill-advised. Many individuals might have skin tags without any underlying metabolic issues, and conversely, some people with insulin resistance may not exhibit any obvious external signs. Therefore, while these observations can be starting points for concern, they are not conclusive proof of insulin resistance and necessitate further investigation.
The Strong PCOS & ED Link
The connection between insulin resistance and conditions like Polycystic Ovary Syndrome (PCOS) in women and erectile dysfunction (ED) in men is notably significant. In men, insulin resistance can negatively impact cardiovascular health and disrupt hormonal equilibrium. It impairs the proper functioning of blood vessels and can alter testosterone levels, thereby increasing the likelihood of experiencing ED. For women, insulin resistance often lies at the heart of PCOS. It can stimulate the overproduction of androgens, leading to a cascade of issues including irregular menstrual cycles, persistent acne, weight gain, and difficulties with fertility. It is important to note that while insulin resistance is a major contributing factor in many cases, not every instance of ED or PCOS is solely attributable to it. Nonetheless, its role in these conditions is substantial and warrants careful consideration.
Accurate Diagnostic Pathways
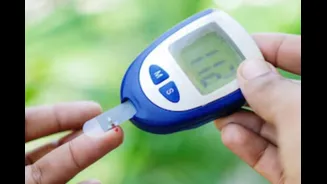
To definitively ascertain whether you are experiencing insulin resistance, a reliable set of diagnostic tests is essential. Commonly employed methods include measuring fasting blood glucose levels, assessing fasting insulin levels, and calculating the HOMA-IR (Homeostatic Model Assessment for Insulin Resistance) score. These provide quantitative insights into how your body is managing blood sugar and insulin. For a more comprehensive evaluation of glucose processing, an Oral Glucose Tolerance Test (OGTT) can be performed. Although the hyperinsulinemic-euglycemic clamp is recognized as the gold standard for measuring insulin sensitivity, its use is primarily confined to research settings due to its complexity. Ultimately, a conclusive diagnosis is best achieved through a holistic approach, integrating a thorough clinical evaluation with the results from these laboratory investigations, rather than relying on any single test.
Reversal Through Lifestyle
The good news is that in its initial phases, insulin resistance can often be significantly improved, and sometimes even reversed, through strategic lifestyle modifications. The cornerstones of this approach include achieving a healthy weight – even a modest loss of 5–10% can make a substantial difference – and incorporating regular physical activity into your routine. Adopting a balanced diet that is rich in protein and fiber further supports metabolic health. Prioritizing adequate sleep and actively managing stress are also vital components. However, for individuals whose insulin resistance has progressed to more advanced stages, such as prediabetes, type 2 diabetes, or severe PCOS, medical intervention might become necessary. In these instances, medications like metformin may be prescribed alongside sustained lifestyle changes. Early intervention remains the most critical factor in managing and potentially overcoming insulin resistance.