The Fit Paradox
A striking case from Hyderabad highlights a concerning trend: a 37-year-old man, rigorously adhering to a healthy lifestyle—daily 5 km runs, a diet free
of junk food, no smoking or drinking, and regular sleep—still required two stents due to significant arterial blockages. This individual exemplified many conventional markers of good health, yet his heart health tells a different story. Dr. Syed Akram Ali, a cardiologist, shared this account, emphasizing that outward fitness can mask deeper vulnerabilities. The man's experience underscores the complexity of cardiovascular health, suggesting that adherence to common lifestyle advice may not offer complete protection against heart disease for everyone.
Unseen Genetic Footprints
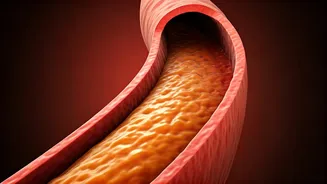
Genetic predispositions and specific biological markers often operate as silent saboteurs of heart health, even when cholesterol levels appear normal. A significant factor is family history; if your father or uncle experienced heart issues at an early age, your own risk of developing cardiovascular disease can multiply by two to three times, irrespective of your current fitness level. Beyond this, Lipoprotein(a), or Lp(a), emerges as a particularly dangerous cholesterol variant. Unlike standard cholesterol tests, Lp(a) is purely genetic and its elevated levels can lead to arterial plaque buildup even when your LDL cholesterol is within the 'normal' range. This particular marker doesn't show up in routine lipid profiles, making it a crucial, yet often overlooked, contributor to heart disease.
Stress, Sleep, and Inflammation
The relentless pressure of a high-stress, corporate lifestyle, combined with inadequate sleep and underlying inflammation, significantly contributes to compromised arterial well-being. It’s a common misconception that intense physical activity like running 5 km daily entirely negates the effects of chronic stress. In reality, stress elevates adrenaline and blood pressure, fostering an inflammatory environment and promoting the formation of micro-plaques within arteries. Furthermore, poor sleep quality—even just six hours coupled with late-night screen use—induces metabolic strain, raising cortisol levels, thickening blood, and destabilizing existing plaques. Hidden inflammation, often measured by C-reactive protein (CRP), is another critical factor. Many individuals who appear physically fit may harbor undetected inflammation, which accelerates artery damage over time, a condition not typically assessed in standard medical checkups.
Beyond Basic Screenings
To truly assess and safeguard cardiovascular health, a comprehensive approach beyond standard tests is essential, particularly for individuals over 25 in India. Dr. Ali recommends a suite of advanced screenings that paint a more complete picture of risk. These include testing for Lipoprotein(a), high-sensitivity C-reactive protein (HS-CRP) to gauge inflammation, ApoB, HbA1c, fasting insulin, Vitamin D levels, and Homocysteine. For those exhibiting symptoms, a TMT (treadmill test) is advised. Crucially, for individuals above 35, a coronary calcium score can detect early plaque buildup even before symptoms manifest. These specialized tests provide deeper insights into genetic predispositions, metabolic health, and inflammatory states, offering a proactive edge in preventing heart disease.