Understanding Gestational Diabetes
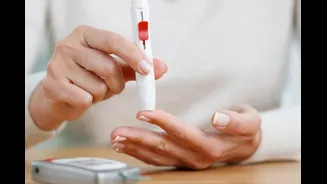
Gestational diabetes (GDM) emerges during pregnancy due to hormonal shifts from the placenta, which aim to support fetal growth but can inadvertently cause insulin resistance, leading to elevated blood
sugar levels. This condition can manifest with symptoms like increased thirst, blurred vision, and frequent urination. Around 60% of women diagnosed with GDM require medical intervention, such as insulin or metformin, to manage their blood sugar effectively. Importantly, GDM is not merely a transient pregnancy-related issue for many; it signals an increased, lifelong risk of developing Type 2 diabetes. Studies indicate that approximately 50% of women who experience gestational diabetes will go on to develop Type 2 diabetes following childbirth. This progression underscores the critical need for awareness and management of GDM not just during pregnancy but also in the years that follow, as it serves as a significant indicator of future metabolic health challenges.
Long-Term Health Risks
The implications of gestational diabetes extend well beyond the delivery room, marking the beginning of a potential lifelong battle with metabolic disorders for a substantial portion of women. Research indicates a stark reality: about half of all women diagnosed with GDM will eventually transition to Type 2 diabetes. This transition is a serious health concern that requires diligent management to prevent further complications. Beyond the personal health risks, GDM is also associated with increased rates of Cesarean section deliveries, emphasizing the broader impact on both maternal and infant outcomes. Contrary to common assumptions, studies have also found a higher incidence of low-birth-weight babies among pregnancies complicated by GDM. Furthermore, the data suggests a genetic predisposition, with approximately one-third of women experiencing GDM having a family history of diabetes, and about 60% of GDM cases occurring in first pregnancies, hinting at a potential link with earlier onset or heightened susceptibility in initial pregnancies.
Post-Partum Surveillance Importance
The findings from recent studies strongly advocate for robust post-partum surveillance for women with a history of gestational diabetes. Experts emphasize that identifying high-risk individuals during pregnancy and implementing structured follow-up care after childbirth are paramount. This proactive approach aims to enable the early detection and timely intervention necessary to prevent or significantly delay the onset of Type 2 diabetes. While the global average prevalence of gestational diabetes is around 15%, some regions, including India, report a higher rate, approximately 22%. A study conducted in Ahmedabad tracked 247 women with known GDM for three years and found that a significant 50% still exhibited elevated blood sugar levels three years post-childbirth, reinforcing the necessity of continuous monitoring and lifestyle adjustments. Effective management strategies, tailored to individual risk factors, are crucial in mitigating the long-term health consequences associated with GDM.