A Vital Partnership
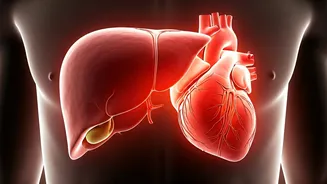
The human body's intricate network relies on the harmonious functioning of its organs, and perhaps no two organs share a more intertwined destiny than
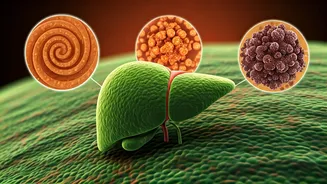
the liver and the heart. While the liver diligently performs essential roles in digestion, metabolism, and detoxification, its health is intrinsically linked to the heart's ability to pump blood efficiently. When the liver falters, this delicate balance is disrupted, placing undue pressure on the cardiovascular system. This essay will delve into how compromised liver function, irrespective of its cause—be it fatty liver disease, hepatitis, cirrhosis, or alcohol-induced damage—can initiate a cascade of changes impacting the heart's workload and the circulatory system's overall health, often in ways that remain concealed during the initial phases of illness.
Circulatory Chaos Unfolds
The liver plays a crucial role in maintaining a steady blood flow, regulating fluid levels throughout the body, managing cholesterol, and controlling inflammation. When liver disease sets in, these vital functions become compromised. This disruption forces the heart to work overtime to sustain circulation, while simultaneously, the body's blood vessels undergo alterations that affect blood pressure regulation and the effective delivery of oxygenated blood to tissues. In advanced stages, particularly with cirrhosis, blood passage through the liver is significantly impeded, leading to increased pressure within the portal vein, a condition known as portal hypertension. Concurrently, peripheral blood vessels dilate, causing a drop in overall blood pressure. The heart's response to this imbalance is to accelerate its pumping rate and increase its force, a sustained effort that, over time, can lead to a weakening of cardiac muscle and a condition termed cirrhotic cardiomyopathy, where the heart loses its capacity to respond adequately to stress.
Fluid Overload Strain
Liver disease frequently triggers the body's tendency to retain excessive amounts of salt and water. This phenomenon results in noticeable fluid accumulation, often manifesting as swelling in the legs, abdomen, and other soft tissues. The presence of this extra fluid places an additional burden on the heart, making its task of circulating blood more arduous and less efficient. In more severe manifestations, this increased fluid volume can contribute to distressing symptoms such as shortness of breath and profound fatigue, further exacerbating the strain on the cardiovascular system and signaling a significant deterioration in overall cardiovascular function.
Co-Existing Risks Magnified
Certain liver conditions, like non-alcoholic fatty liver disease (NAFLD), often occur alongside other significant health issues such as diabetes, obesity, elevated cholesterol levels, and hypertension. These co-existing conditions are already recognized as major contributors to the development of heart disease. Moreover, the chronic inflammation that is a hallmark of liver damage can independently heighten the risk of developing atherosclerosis—the hardening and narrowing of arteries—and other serious cardiac complications, creating a complex web of interconnected health challenges that demand comprehensive management.