A Surprising Discovery
Consider a 48-year-old man, the epitome of good health. He maintained a lean physique at 174 cm and 67 kg, swam daily, and boasted an impressively low
resting heart rate of around 48 beats per minute, indicating a robust heart. He was a non-smoker, favored whole foods in his diet, and had no obvious health concerns. His voluntary decision to undergo routine heart function tests, including ECG, echocardiogram, and stress tests, revealed no issues. However, a calcium score test, a CT scan assessing calcified plaque in the arteries, flagged a concern with a score of 30, significantly above the safe range of 1-10. While his standard lipid profile showed a low LDL cholesterol below 60 mg/dL, a subsequent Lipoprotein(a) or Lp(a) test revealed an elevated level of 70 mg/dL, far exceeding the normal threshold of less than 30 mg/dL. This finding pointed to a problematic component of cholesterol that adheres to artery walls, escalating the risk of heart disease and stroke. Notably, individuals of Indian and South Asian descent exhibit a higher prevalence of elevated Lp(a), with approximately 25% of this population group having heightened levels, making it a pertinent concern for many.
Understanding Lp(a)
Lipoprotein(a), or Lp(a), is a unique type of cholesterol particle circulating in our bloodstream. Its presence and levels are largely dictated by our genetic makeup, meaning it's something we inherit rather than acquire through lifestyle choices. What distinguishes Lp(a) from typical cholesterol particles like LDL is the addition of a special protein, apolipoprotein(a). This extra protein alters the particle's behavior within the body, rendering it more detrimental to our cardiovascular system than ordinary LDL cholesterol. Consequently, even individuals who meticulously adhere to a healthy diet and exercise regimen, maintaining excellent standard cholesterol readings, can still harbor elevated Lp(a) levels solely due to their inherited DNA. This inherent characteristic makes Lp(a) a formidable and often overlooked risk factor for heart disease, as conventional methods for managing cholesterol are often ineffective against it.
How Lp(a) Harms Arteries
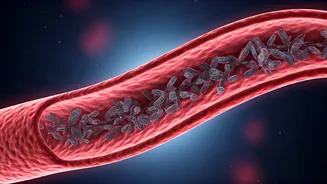
Lp(a) contributes to heart disease through a multi-faceted process. Initially, much like LDL, it transports cholesterol directly into the artery walls. Over time, this cholesterol accumulation leads to the formation of fatty deposits, commonly known as plaques. These plaques progressively narrow the arteries, impeding blood flow and consequently increasing the likelihood of experiencing chest pain, heart attacks, and other cardiovascular complications. Furthermore, the apolipoprotein(a) component imbues Lp(a) with a sticky and inflammatory nature. This property triggers irritation within the delicate lining of our blood vessels, accelerating the growth of these detrimental plaques. The plaques influenced by Lp(a) also tend to be inherently less stable, making them more prone to sudden rupture, which can precipitate acute cardiac events. Adding to its danger, Lp(a) interferes with the body's natural mechanisms for dissolving blood clots. This disruption allows blood clots to form more readily and persist for longer durations, significantly elevating the risk of both heart attack and stroke. These combined effects explain why Lp(a) poses a threat even to individuals who outwardly appear in peak physical condition.
Who Needs Testing?
Identifying elevated Lp(a) levels is straightforward, requiring a simple blood sample. Since these levels tend to remain stable throughout a person's life, repeat testing is usually not necessary, and the test itself is quite affordable. The decision to test for Lp(a) becomes particularly important for individuals with a history of heart disease despite having normal cholesterol levels, those with exceptionally high LDL cholesterol, or if familial hypercholesterolemia is suspected. It is also recommended for patients who experience recurrent cardiac events even after undergoing treatment. A family history of premature heart disease or stroke is another strong indicator for considering an Lp(a) test, as it can reveal a genetic predisposition that may not be apparent from other risk factors. Early detection through this test can empower individuals and their healthcare providers to implement more targeted strategies for cardiovascular risk management.
Managing High Lp(a)
Standard cholesterol-lowering medications, such as statins, are highly effective in reducing LDL cholesterol and are crucial for preventing heart attacks and strokes. However, research indicates that statins might paradoxically increase Lp(a) levels by approximately 10–20%. Importantly, this slight increase does not negate the significant heart-protective benefits of statins, so doctors generally do not discontinue statins solely based on a higher Lp(a). When Lp(a) levels are mildly elevated, the concern is less pronounced. However, when Lp(a) is considerably high, it acts as a significant risk amplifier, similar to having ample fuel for a fire. In such cases, healthcare providers aim to drastically lower LDL cholesterol, targeting levels below 30 mg/dL. To achieve this, cardiologists might combine low-dose statins with PCSK9 inhibitors, currently the most potent approved medications for Lp(a) reduction, which can lower LDL by up to 70% and Lp(a) by roughly 20–30%. Promisingly, an oral daily pill is under clinical trial, showing potential to reduce Lp(a) by 65–85% and is anticipated for availability by late 2026 or early 2027. Until then, aggressive management of other modifiable risk factors, including strict LDL targets, blood pressure control, diabetes prevention, smoking cessation, and regular exercise, remains paramount.