Study's Skeptical Findings
A comprehensive umbrella review, analyzing nearly 13,000 patients across numerous studies and trials up to November 2025, has cast doubt on the extent
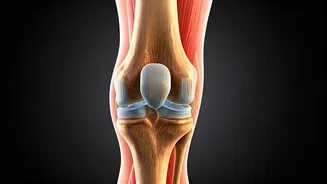
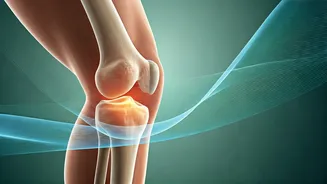
of exercise benefits for osteoarthritis. This analysis, published in February 2026, specifically examined exercise's impact on hip, hand, knee, and ankle osteoarthritis. When compared against various interventions including no treatment, placebo, patient education, manual therapy, NSAIDs, and even surgical options like osteotomy and joint replacement, exercise demonstrated only modest and often transient pain reduction, typically between 6 to 12 points on a 100-point scale. For knee osteoarthritis, the evidence was particularly weak and short-lived, with negligible effects for hip osteoarthritis and small benefits for hand osteoarthritis. Crucially, exercise did not significantly outperform other conservative treatments like patient education or NSAIDs in improving function, and in some instances, surgical interventions provided superior long-term outcomes. The study's authors concluded that the evidence for exercise's effectiveness is largely inconclusive and questioned its universal promotion as a sole first-line treatment.
Reframing Expectations
While the study's findings may seem discouraging, experts like Dr. Sandeep Nagar, a Rheumatology Consultant, urge a re-evaluation of expectations rather than a dismissal of exercise. He highlights that modern pain management prioritizes enhanced functional capacity over achieving complete pain elimination. A reduction of 7-15 points on a 100-point pain scale is often considered a clinical success, as it enables individuals to perform more daily activities despite some lingering discomfort. This perspective shift acknowledges that even moderate pain relief can lead to significant improvements in quality of life, such as increased walking tolerance, better sleep patterns, and a reduction in the fear of movement. Furthermore, exercise has biological benefits, including activating the body's natural pain-relieving systems, which can elevate pain thresholds over time. Therefore, the clinical success of exercise is measured not just by a numerical pain score, but by its ability to restore and maintain a person's ability to engage in life.
Exercise's Enduring Value
Despite the study's quantitative findings, experts maintain that exercise should remain a foundational element in osteoarthritis management due to its unique long-term benefits. Unlike medications, which primarily mask symptoms and carry potential systemic risks such as gastric and renal issues with NSAIDs, or dependency with opioids, exercise directly addresses biomechanical dysfunction and builds resilience. Dr. Nagar emphasizes that consistent physical activity strengthens supporting muscles, improves joint mechanics, and can even support cartilage health, offering structural advantages that pharmaceuticals cannot provide. Moreover, the comparative cost-effectiveness is significant; while medications incur ongoing expenses and potential long-term health complications, regular exercise has a superior safety profile and can potentially save substantial amounts on healthcare costs over a lifetime by delaying or reducing the need for surgery. Although exercise is dose-dependent and requires consistent participation, its risk-benefit ratio remains highly favorable, especially when approached strategically.
Study Limitations Unpacked
The umbrella review's conclusions, while noteworthy, are subject to several significant limitations that may have understated exercise's true impact. One major issue is the collective analysis of diverse exercise modalities, ranging from strength training and aerobic workouts to stretching and aquatic exercises. These different forms of activity possess varying intensities and physiological effects, and grouping them may have obscured the specific benefits of more potent exercises like resistance and aerobic training. Additionally, the review did not differentiate between supervised and unsupervised exercise programs; supervised sessions typically yield better adherence, technique, and progression, leading to superior outcomes. The study durations were also often short, typically around 12 weeks, which might not capture the cumulative, long-term benefits that can accrue from consistent, lifelong engagement with exercise. Finally, the exact 'dose' and intensity of exercise were not always fully accounted for, meaning that some participants might not have met the recommended 150 minutes of moderate-intensity exercise per week, thus not achieving optimal results that could have been attributed to exercise efficiency rather than its inherent limitations.
Beyond Pain Relief
It's crucial to recognize that the benefits of exercise for individuals with osteoarthritis extend far beyond merely alleviating joint pain and improving immediate function. The comprehensive review acknowledged these broader, secondary health advantages, which play a vital role in overall well-being and resilience. Regular physical activity is a cornerstone of effective weight management, a critical factor in reducing stress on weight-bearing joints like the knees and hips. Furthermore, exercise has a well-documented positive impact on mental health, contributing to improved mood and reducing symptoms of depression and anxiety, which often co-occur with chronic pain conditions. On a physiological level, consistent exercise enhances cardiovascular health, lowers the risk of developing type 2 diabetes, and has been associated with a reduced risk of certain cancers. These systemic benefits, when considered in shared decision-making between patients and healthcare providers, underscore the holistic value of exercise, reinforcing its position as an indispensable component of comprehensive osteoarthritis care, even when its direct impact on pain scores might appear modest.
Protecting Your Joints
For individuals managing osteoarthritis and engaging in exercise, prioritizing joint protection through proper warm-up and cool-down routines is paramount. Dr. Nagar emphasizes the importance of preparing the body for physical activity and aiding its recovery. A warm-up session, lasting 5 to 10 minutes, should involve light aerobic activities such as brisk walking or cycling, combined with dynamic movements like leg swings, arm circles, and walking lunges. These movements increase blood flow to the muscles, improve joint mobility, and prepare the musculoskeletal system for exercise. Following the workout, a cool-down period of another 5 to 10 minutes is essential. This involves gradually decreasing the intensity of activity to allow the heart rate to return to normal, followed by static stretches. Holding stretches such as those for the hamstrings or quadriceps for 10 to 30 seconds helps to improve flexibility and reduce muscle soreness. Implementing these structured routines can significantly enhance the safety and effectiveness of exercise, minimizing the risk of aggravating existing pain and maximizing the long-term benefits of physical activity.