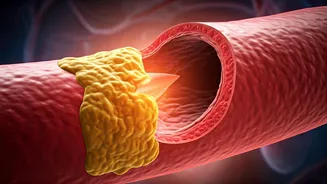
Arterial Damage Begins
Contrary to popular belief, a heart attack isn't a sudden, unannounced catastrophe. The journey truly begins with subtle damage to the inner lining of
your arteries, a living tissue that can be compromised over time. Factors like elevated blood pressure, high cholesterol levels, the habit of smoking, and unmanaged diabetes are key culprits that initiate this wear and tear. As your body attempts to repair this damage, it unfortunately lays down fatty substances on the artery walls. This accumulated material gradually hardens, forming what is known as plaque, a process called atherosclerosis. Astonishingly, this insidious development can commence as early as your twenties, silently progressing for decades before any noticeable symptoms emerge.
Plaque Buildup and Narrowing
As atherosclerosis advances, the accumulation of plaque within the arteries leads to a significant narrowing of these vital passageways. This constriction impedes the smooth flow of blood throughout your circulatory system, making it more challenging for your body to receive the oxygen-rich blood it needs. What's particularly concerning is that during this phase of arterial narrowing, the majority of individuals remain completely asymptomatic. The arteries may become substantially constricted, perhaps by as much as 70-80%, yet you might feel perfectly fine, lulling you into a false sense of security. This lack of overt symptoms makes the silent progression of heart disease all the more perilous, as the damage continues unchecked beneath the surface.
The Critical Rupture Event
While a narrowed artery is a concern, the true trigger for a heart attack often lies in the instability of the plaque itself. Not all plaque is created equal; softer, more fragile plaques are more prone to sudden rupture. When such a rupture occurs, the body's immediate response is to dispatch platelets and other clotting factors to the site to staunch the bleeding and attempt repairs. This inflammatory response, however, can be a double-edged sword. A significant blood clot can form rapidly at the ruptured site, potentially completely blocking the already narrowed artery. This abrupt blockage halts blood flow to a segment of the heart muscle, depriving it of oxygen and leading to tissue damage – the hallmark of a heart attack.
Accelerating Factors and Warning Signs
Several lifestyle and metabolic factors can accelerate the rate at which plaque forms and increase the likelihood of its rupture. High levels of LDL (bad) cholesterol, poorly controlled high blood pressure, persistent smoking, diabetes, chronic stress, lack of regular physical activity, and carrying excess body weight all contribute to a more aggressive form of atherosclerosis. These detrimental influences often operate without obvious symptoms, quietly degrading arterial health until a critical event occurs. However, the body may offer subtle warnings that are easily overlooked. These can include unexplained fatigue, chest discomfort that arises during exertion, shortness of breath, and radiating pain in the upper back, arms, or jaw. Recognizing and heeding these signs is crucial for timely medical intervention.
Prevention and Management Strategies
Since a heart attack is the result of a prolonged pathological process rather than an instant occurrence, preventative measures are highly effective. By actively managing the underlying risk factors, individuals can significantly slow down plaque formation and maintain healthier arteries. This involves maintaining healthy blood pressure and cholesterol levels, engaging in regular exercise, adopting a nutritious diet, and refraining from smoking. Regular health check-ups are essential for monitoring key indicators such as blood pressure, cholesterol, and blood sugar levels. Early detection and consistent management of these risk factors are paramount in reducing the likelihood of a heart attack and preserving cardiovascular health over the long term.