Understanding Ozempic's Mechanism
Ozempic, a medication primarily recognized for its role in managing type 2 diabetes, has garnered significant attention for its potential in aiding weight
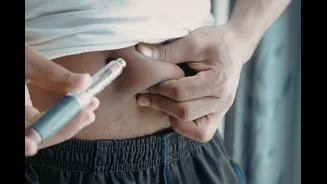
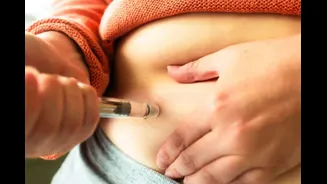
loss. Its efficacy is rooted in its interaction with the GLP-1 hormone pathway, a crucial system that governs blood sugar regulation and appetite control. Semaglutide, the active component in Ozempic, works by mimicking the effects of this hormone, thereby influencing satiety and insulin secretion. However, the journey of Ozempic from a diabetes treatment to a widely discussed weight management tool underscores the complex physiological responses it can elicit. The drug's intended purpose is to help individuals maintain stable blood sugar levels and avoid the long-term health complications associated with diabetes. For those prescribed Ozempic, especially for weight management, continuous medical oversight is paramount to ensure safety and monitor its impact on the body over time. This careful administration is key to harnessing its benefits while mitigating potential risks.
The Science Behind Varied Responses
A recent scientific investigation has shed light on the fundamental reasons why Ozempic does not produce a uniform effect across all users. This groundbreaking study, published in Genome Medicine, delved into the intricacies of the GLP-1 signaling pathway, observing variations in both human and mouse subjects, and corroborating findings with existing clinical trial data. The research pinpointed that individuals possess differing levels of sensitivity or unique signaling patterns within this critical pathway. These biological discrepancies mean that the drug's intended impact on appetite suppression and insulin release can be significantly altered from one person to another. Consequently, the observed effectiveness of Ozempic, including its ability to facilitate dramatic weight loss or improve diabetes markers, can range from substantial to minimal, even with consistent adherence to the prescribed regimen. This scientific revelation underscores the necessity for a tailored approach to Ozempic usage, moving away from a one-size-fits-all model.
Individual Factors Influencing Efficacy
Several underlying biological factors contribute to the divergent responses individuals experience with Ozempic, explaining why some achieve remarkable results while others see limited benefits. Genetic predispositions play a significant role, as inherent variations in an individual's DNA can alter how their body processes and responds to semaglutide. Furthermore, the complex interplay between the gut and the brain, often referred to as gut-brain signaling, can be a critical determinant of Ozempic's effectiveness. Issues within this communication network may impede the drug's ability to signal satiety or regulate appetite. Chronic inflammation within the body also presents a variable that can influence how the medication functions. Lastly, advanced metabolic dysfunction, where the body's metabolic processes are impaired, can affect how Ozempic is absorbed, utilized, and ultimately, its overall impact on the user. These multifaceted elements necessitate a personalized assessment by healthcare professionals.
Personalized Treatment for Ozempic
The nuanced understanding of Ozempic's varied efficacy derived from recent studies points towards an essential shift in its application: personalized treatment strategies. For patients, this means establishing realistic expectations, which can only be achieved through open and thorough consultations with their healthcare providers. It is imperative to recognize that while Ozempic is a potent medication, its effectiveness is not guaranteed to be universal. Therefore, constant medical supervision is non-negotiable, ensuring patient safety by monitoring for any adverse effects or unexpected physiological responses. This vigilance allows for timely adjustments to dosage, administration timing, or even the exploration of alternative treatment avenues if a patient proves to be a non-responder. The future of weight-loss drugs, including those in the GLP-1 class, is leaning towards precision medicine, where treatments are custom-designed based on an individual's unique biological profile and health status.