Sciatica's Subtle Signals
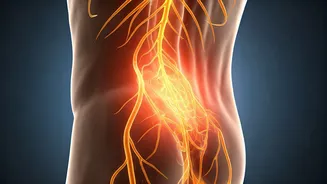
Sciatica is far more than a mundane backache; it’s your body’s urgent communiqué regarding an issue with the critical sciatic nerve, the longest in the human
anatomy. This nerve originates in the lower spinal region and extends through the hips, buttocks, and all the way down the legs to the feet. When external pressures, such as from a herniated disc, bone spur, or muscle constriction, affect this nerve, it triggers a cascade of uncomfortable sensations. Ignoring these initial indicators, which often manifest as pain radiating down the leg, tingling, or a noticeable decrease in muscle strength, can unfortunately transform a manageable condition into a persistent, life-altering disability. Early recognition and understanding of these warning signs are paramount for initiating timely and effective treatment, thereby safeguarding against potential long-term nerve deterioration.
Recognizing Red Flags
The tell-tale signs of sciatica typically extend beyond the lumbar region, traveling downwards into the leg. As the sciatic nerve plays a dual role in both sensation and motor function, the specific symptoms can vary significantly from one individual to another. Being attuned to these early warning indicators is crucial for prompt medical attention. Common manifestations include a burning or shooting pain that emanates from the lower back and descends into the thigh or calf, often described as feeling like an electric shock. You might also experience a sensation of numbness or 'pins and needles' in your foot or toes, as if that part of your limb has gone to sleep. Another sign is observable muscle weakness, which could manifest as difficulty lifting the front of your foot or feeling unstable when attempting to stand or walk. Furthermore, certain actions can exacerbate the pain, such as prolonged sitting, coughing, or sneezing, which can trigger sharp, intense discomfort. Experts advise seeking medical help if this radiating pain persists for over three days, especially if accompanied by numbness or weakness, as early imaging and evaluation are vital to prevent irreversible nerve damage.
The Peril of Postponement
The sciatic nerve functions like a vital communication highway for your legs, transmitting crucial signals for movement and sensory feedback. When this pathway is obstructed, for instance, by a disc bulge or a bony protrusion, it leads to immediate inflammation and distress. Delaying treatment allows this compression to persist, effectively starving the nerve of essential blood flow. Over time, this sustained lack of oxygen can lead to the degradation and even death of nerve fibers, a condition known as permanent neuropathy, where symptoms like persistent numbness and muscle weakness become irreversible. In more severe, albeit rare, instances, extreme nerve compression can culminate in Cauda Equina Syndrome, a critical medical emergency requiring immediate intervention. This syndrome can result in a loss of bladder and bowel control and, without swift treatment, can lead to permanent paralysis. Early intervention is the most effective strategy to halt this degenerative process before irreparable damage takes hold.
Accelerating Your Recovery
Encouragingly, approximately 90% of individuals experiencing sciatica can achieve recovery without resorting to surgical procedures, provided they seek timely medical assistance. A proactive approach, incorporating specialized physical therapy, strategic movement, and ergonomic adjustments, can significantly expedite the healing journey. Specialized physical therapy employs targeted exercises and techniques designed to decompress the spine, improve mobility, and rebuild muscular strength, particularly in the core, which acts as a natural support system for the spine, reducing pressure on the discs. Contrary to older advice, complete bed rest is often detrimental; while a short period of rest may be beneficial during an acute episode, prolonged inactivity can stiffen muscles. Regular walking, however, promotes blood circulation to the nerves, which is vital for healing. Moreover, addressing repetitive poor movement patterns is crucial. Making ergonomic modifications, such as adjusting desk heights, using lumbar support, and employing proper lifting techniques, can prevent the ongoing micro-trauma that irritates the nerve. While surgery remains an option for extreme cases, non-surgical methods are highly effective for most patients, emphasizing the spine's need for movement and proper rehabilitation for natural healing.