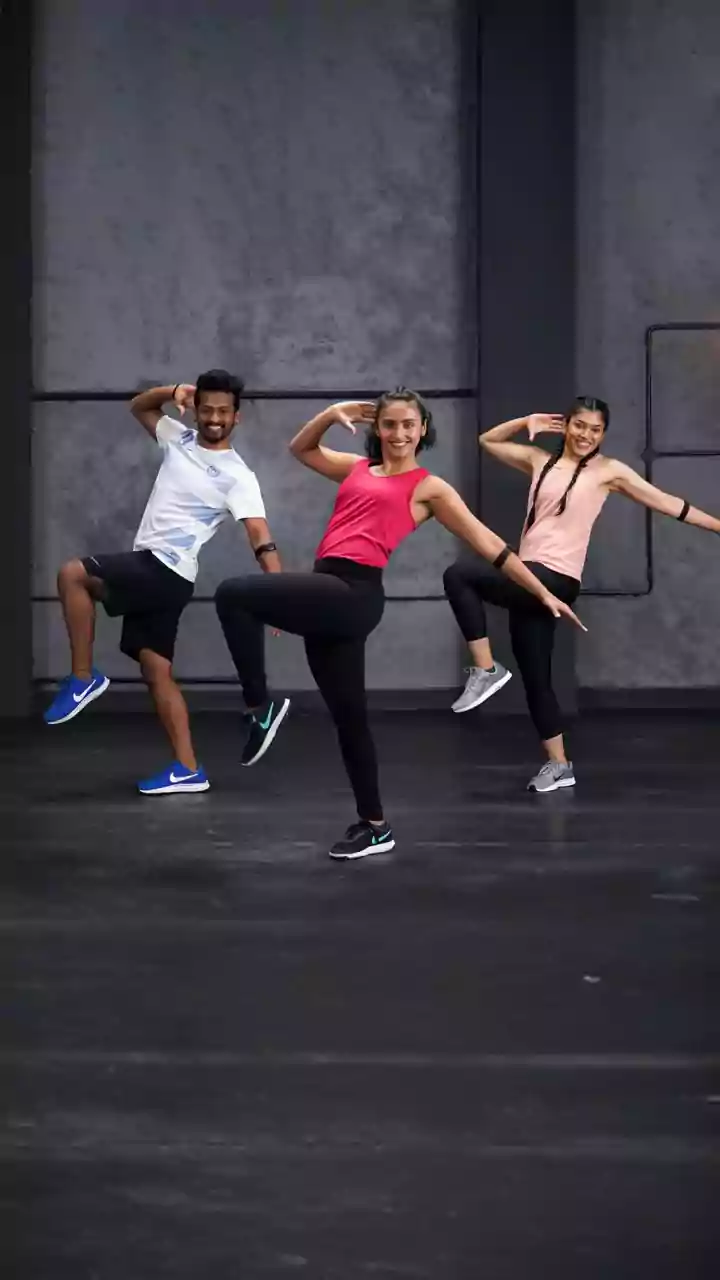The Stress-Fatty Liver Link
Many individuals believe that Non-Alcoholic Fatty Liver Disease (NAFLD), now also termed Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD),
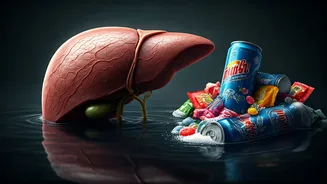
is primarily a consequence of poor dietary habits, excessive sugar intake, or heavy alcohol consumption. However, a growing number of patients, even those who maintain a healthy lifestyle, exercise regularly, and abstain from alcohol, are presenting with this diagnosis. Their medical scans reveal an accumulation of fat in the liver, a perplexing situation for both the patients and their physicians. This scenario points to a less recognized, yet significant, contributor: chronic stress. The constant pressure and demands of modern professional life can elevate cortisol, the body's primary stress hormone, which in turn can signal the liver to store excess fat, thereby contributing to the development of NAFLD/MASLD, even in individuals who appear to be metabolically healthy on the surface.
Cortisol's Liver Impact
The persistent activation of the body's stress response system, triggered by demanding careers, leads to chronically elevated levels of cortisol. This hormone, while essential for short-term survival and energy mobilization, has detrimental long-term effects when continuously present. Specifically, elevated cortisol influences how the liver processes and stores energy. It promotes gluconeogenesis, the creation of glucose from non-carbohydrate sources, and encourages the conversion of excess energy into fat. This fat, in turn, gets deposited in the liver, contributing to the steatosis, or fatty buildup, characteristic of NAFLD/MASLD. It's a biological mechanism where the body, perpetually anticipating a 'fight or flight' scenario, prioritizes energy storage, inadvertently leading to a health crisis in the liver, even in the absence of typical risk factors.
Breaking the Cycle
Understanding the role of cortisol in NAFLD/MASLD is the first step towards breaking the cycle of stress-induced liver fat accumulation. Hepatologists emphasize that managing chronic stress is as crucial as dietary adjustments for individuals at risk or already diagnosed. This involves adopting a multifaceted approach to well-being. Strategies can include incorporating mindfulness practices, engaging in regular physical activity that is enjoyable and sustainable, ensuring adequate sleep, and seeking social support. Furthermore, professionals need to critically evaluate their work-life balance and explore methods to reduce workplace pressures, such as setting boundaries, delegating tasks, and practicing time management techniques. By actively mitigating stress and its hormonal consequences, individuals can help reverse or prevent the progression of fatty liver disease, fostering a healthier hepatic environment and overall well-being.