The Promise of Amyloid Clearance
For a long time, the scientific community and families affected by Alzheimer's disease have sought a way to halt or significantly slow the progression
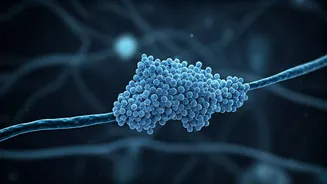
of memory loss. A new wave of medications emerged with a targeted approach: reducing amyloid-beta protein, which accumulates in the brain and forms harmful plaques characteristic of Alzheimer's. The fundamental theory behind these treatments, such as lecanemab and donanemab, is that by clearing these amyloid plaques, the underlying disease process can be disrupted, thereby preserving cognitive function. These drugs, designed as monoclonal antibodies, work by binding to amyloid proteins and facilitating their removal from brain tissue. Crucially, brain imaging studies have confirmed that these treatments do indeed lead to a reduction in amyloid plaque burden, validating the biochemical mechanism they employ. This success at the molecular level, however, leads to the more critical question: does this plaque reduction translate into tangible, observable benefits for patients in their day-to-day lives, such as improved memory recall or enhanced ability to perform daily tasks?
Cochrane Review Findings
A comprehensive and rigorous review, conducted by the Cochrane organization, has thoroughly analyzed the available evidence from 17 distinct clinical trials involving over 20,000 participants. This extensive data set represents some of the most robust scientific information currently accessible on the topic of these amyloid-targeting therapies. The review's conclusions, however, present a sobering perspective. It found that while the drugs do reduce amyloid plaques, the resulting improvements in memory and cognitive abilities were statistically minor, falling short of what would be considered clinically significant for the majority of patients. The review indicated that changes in dementia severity were negligible or showed no meaningful improvement, and enhancements in daily functioning were either slight or non-existent. In essence, the drugs may demonstrate a slowdown in decline when measured by specific metrics, but this effect is often too subtle for individuals and their caregivers to perceive in their daily experiences. The disparity between statistically measurable changes and genuinely felt benefits is a key area of concern and disappointment within the Alzheimer's research community.
Risks and Treatment Burden
It is essential to acknowledge that no medical intervention is entirely without potential downsides, and these novel Alzheimer's treatments are no exception. The Cochrane review specifically highlighted an increased incidence of side effects related to the brain. These adverse events, collectively known as amyloid-related imaging abnormalities (ARIA), can manifest as brain swelling (ARIA-E) or small brain bleeds (ARIA-H). The data suggests that for every thousand individuals receiving these medications, approximately one hundred more experienced brain swelling compared to a control group not receiving the treatment. Beyond these physiological risks, the treatment regimen itself imposes a considerable burden. Patients require regular infusions, typically administered in a hospital or clinic setting every few weeks. For elderly individuals, who often constitute the primary patient population for Alzheimer's, and their families, the logistical, physical, and emotional demands of these frequent medical appointments can be substantial and taxing, raising questions about the overall sustainability and feasibility of long-term treatment.
Expert Disagreements Emerge
The implications of these review findings have sparked a notable divergence of opinion among medical professionals and researchers. Some experts contend that the initial enthusiasm surrounding these drugs has been disproportionate to their actual clinical impact, with one of the study's authors, Edo Richard, suggesting that the demanding nature of the treatment might outweigh its limited benefits. Conversely, other specialists advocate for a more nuanced interpretation of the data. For instance, Bart De Strooper has argued that the newer medications do offer 'modest but real' improvements, particularly when administered in the earlier stages of the disease. This debate brings to the forefront a fundamental question: In the context of a progressive and irreversible condition like Alzheimer's, do even small improvements hold significant value? For some families, securing even a few additional months of slower disease progression can be profoundly meaningful. However, for others, the combination of high costs, considerable effort, and the inherent risks associated with the treatment may render it an unappealing or impractical option. The divided perspectives underscore the complexity of evaluating these therapies.
Patient and Family Guidance
The recent research and expert discussions should not be misconstrued as an indictment of all treatment possibilities for Alzheimer's disease. Instead, they serve as a crucial recalibration of expectations for patients and their loved ones. It is vital to understand that these drugs are not a definitive cure for Alzheimer's; rather, they are designed to potentially modify the disease's progression. Any benefits observed are likely to be modest and may not be universally experienced. Furthermore, the treatment journey is characterized by significant time commitment, financial investment, and the necessity of ongoing medical supervision and monitoring for potential side effects. Consequently, decisions regarding the initiation or continuation of these therapies should be deeply personalized, taking into account the individual's specific health profile, disease stage, and personal values. Crucially, these decisions must be made in close consultation with qualified healthcare professionals, such as neurologists, who can provide tailored advice based on a comprehensive assessment of the patient's circumstances.