Endometriosis: A Persistent Condition
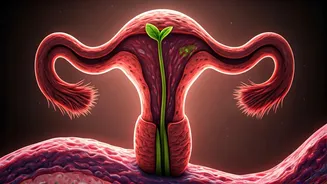
Endometriosis is a chronic health issue where tissue similar to the uterine lining grows outside the uterus, commonly affecting ovaries, fallopian tubes,
and the pelvic lining. This misplaced tissue reacts to hormonal shifts during the menstrual cycle, thickening, shedding, and bleeding. Since this blood and tissue cannot leave the body, it gets trapped, leading to inflammation, swelling, the formation of scar tissue, and sometimes adhesions that can bind organs together. This process is the root cause of severe menstrual pain, pelvic discomfort, and can pose challenges for fertility. The exact origins of endometriosis remain under investigation, with theories like retrograde menstruation (menstrual blood flowing backward into the pelvic cavity), immune system deficiencies, genetic factors, and hormonal imbalances, particularly estrogen dominance, being explored. It's a complex interplay of factors, leading to varied symptom severity among individuals.
Pregnancy's Hormonal Shift
During pregnancy, a woman's body undergoes significant hormonal adjustments. Ovulation ceases, and menstruation stops, leading to a sustained increase in progesterone levels and a more balanced estrogen profile. These hormonal changes directly influence endometriosis, a condition highly sensitive to hormonal fluctuations. Because the inflammatory and painful symptoms of endometriosis often peak before menstruation, the absence of periods during pregnancy can lead to a noticeable reduction in pain and discomfort for many women. This temporary reprieve is due to the suppression of the menstrual cycle, which is a primary driver of symptom exacerbation in endometriosis. The elevated progesterone can also play a role in calming the inflamed tissues.
Temporary Relief, Not a Cure
While pregnancy can offer welcome symptom relief, it is crucial to understand that this effect is temporary and does not constitute a cure for endometriosis. The underlying endometrial-like lesions do not disappear simply because a woman is pregnant. Once menstruation resumes after childbirth, the symptoms of endometriosis typically return. In some cases, discomfort can persist even throughout pregnancy, potentially caused by adhesions, scar tissue, or the growing uterus pressing on other abdominal organs. Organizations like the American College of Obstetricians and Gynecologists emphasize that endometriosis is a chronic condition requiring appropriate medical management. This often involves a multi-faceted approach, which may include hormonal therapies, pain management strategies, lifestyle modifications, and sometimes surgical interventions, tailored to the individual's specific condition.
Beyond Pregnancy: Management Strategies
The notion that pregnancy serves as a treatment for endometriosis can be misleading and problematic, especially given that endometriosis itself can complicate achieving pregnancy for some individuals. Experts clarify that while pregnancy might alleviate symptoms for certain women, it is not a definitive solution. Managing endometriosis effectively typically involves a comprehensive strategy that goes beyond pregnancy. This often includes targeted hormonal treatments to regulate the menstrual cycle and reduce lesion growth, robust pain management plans to address discomfort, and significant lifestyle adjustments that can help mitigate inflammation and improve overall well-being. For more advanced or persistent cases, surgical options to remove or destroy ectopic endometrial tissue may be considered. These approaches aim to manage the chronic nature of the disease and improve quality of life.