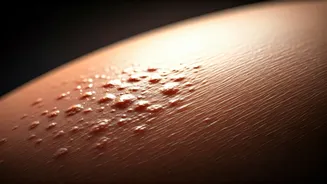
Eczema's Mark
Eczema, a chronic inflammatory skin condition, often raises concerns about its potential to leave permanent scars. While eczema itself isn't typically
characterized by deep, scar-forming wounds like injuries, its persistent nature and the intense itching associated with it can lead to secondary changes in the skin's appearance and texture over time. The constant scratching and rubbing, often a subconscious reaction to the discomfort, can disrupt the skin's natural barrier. This repeated trauma can cause thickening of the skin, a condition known as lichenification, which may appear darker and feel rougher than the surrounding skin. In some instances, particularly with severe or infected eczema flares, hyperpigmentation (darkening of the skin) or hypopigmentation (lightening of the skin) can occur as the skin tries to repair itself. These pigmentary changes, while not true scars in the sense of a deep tissue injury, can be persistent and affect the skin's overall aesthetic. Understanding that these changes are often a result of the management of eczema, rather than the condition itself, is crucial for effective skin care.
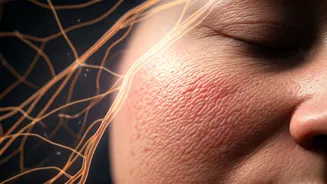
Skin Texture Alterations
The chronic inflammation and scratching inherent to eczema can significantly alter the skin's texture, presenting a different kind of lasting effect. When eczema flares up, the skin becomes inflamed, red, and intensely itchy. The natural urge to scratch, even if resisted, can lead to micro-tears and damage to the epidermal layer. Over prolonged periods, this repetitive scratching can cause the skin to become thicker and leathery, a phenomenon called lichenification. This thickened skin often loses its suppleness and can appear more pronounced or raised compared to unaffected areas. Furthermore, the compromised skin barrier, a hallmark of eczema, makes the skin more vulnerable to environmental irritants and allergens, perpetuating a cycle of inflammation and further textural changes. While not always considered 'scars' in the traditional sense, these textural alterations can be quite noticeable and persistent, impacting the smoothness and feel of the skin. Proper management of eczema aims to break this cycle by reducing inflammation and preventing scratching, thereby helping to preserve the skin's natural texture.
Healing and Pigmentation
The skin's response to inflammation and injury, including that caused by eczema, often involves changes in pigmentation as part of the healing process. When eczema flares, the skin's cells responsible for producing melanin (melanocytes) can become overactive or underactive in their attempt to repair the damaged tissue. This can result in post-inflammatory hyperpigmentation, where the affected areas appear darker than the surrounding skin, or post-inflammatory hypopigmentation, where they become lighter. These pigmentary changes are a common occurrence after any form of skin inflammation, not exclusive to eczema. The severity and duration of the eczema flare-up, as well as individual skin types, play a significant role in the extent of pigmentation changes. While these dark or light spots are often temporary and can fade over months or even years, they can sometimes be quite persistent. Sun exposure can also exacerbate hyperpigmentation, making it appear more prominent. Therefore, protecting the skin from the sun with broad-spectrum sunscreen is an important step in managing these lingering pigmentary effects and promoting an even skin tone.