Lactose Intolerance's Role
Persistent heartburn can be baffling, especially when antacids offer little relief. Dr. Saurabh Sethi, a gastroenterologist with Harvard and Stanford training,
points to lactose intolerance as a significant yet frequently missed contributor. A substantial portion of the global population, nearly two-thirds, experiences some degree of difficulty digesting lactose. When this sugar isn't broken down effectively, it can lead to an uncomfortable buildup of gas and bloating within the abdomen. This internal pressure can then exacerbate acid reflux symptoms, pushing stomach contents back up into the esophagus, particularly in individuals already prone to such issues. Therefore, if your heartburn lingers despite consistent antacid use, assessing your body's response to dairy might be a crucial next step in pinpointing the true source of your discomfort, moving beyond symptom management to address the underlying digestive inefficiency.
The H. pylori Connection
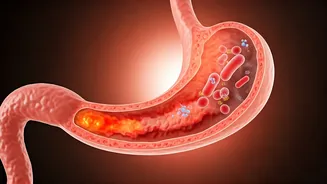
Another frequently overlooked factor contributing to stubborn heartburn is an infection by a common stomach bacterium known as Helicobacter pylori, or H. pylori. This microorganism is surprisingly prevalent, affecting a large segment of the world's population. Its presence can trigger inflammation within the stomach lining, a condition called gastritis. Beyond inflammation, H. pylori can also subtly alter the way stomach acid is produced and regulated. These changes in acid dynamics are believed to contribute to various upper gastrointestinal discomforts, including symptoms that mimic or directly cause acid reflux. Dr. Sethi emphasizes that while not every case of heartburn is due to these two factors, they represent significant areas to investigate when symptoms persist, advocating for a thorough evaluation to treat the root cause rather than just masking the effects.
Clinical Recommendations & Next Steps
When facing persistent heartburn, Dr. Sethi outlines a pragmatic approach based on suspected causes. If lactose intolerance is the likely culprit, his recommendation involves a practical trial: temporarily switching to lactose-free dairy alternatives or plant-based milk substitutes. By observing whether symptoms improve with this dietary change, patients can gain valuable insight into the role of lactose. For suspected H. pylori infections, the gastroenterologist advocates for non-invasive diagnostic methods. These typically include a breath test or a stool test, which are convenient and effective in detecting the bacterium. Should these tests confirm the presence of H. pylori, appropriate medical treatment can then be initiated to eradicate the infection, thereby addressing a key driver of persistent reflux and other gastrointestinal woes. This patient-centric approach prioritizes identifying the specific issue for targeted and effective relief.