The Silent Cascade
Rajesh Mehta, a 52-year-old Pune resident, diligently managed his diabetes with medication, diet, and regular doctor visits. Despite his efforts, he developed
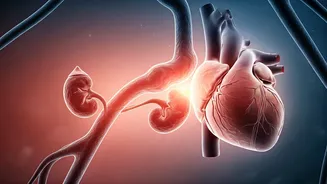
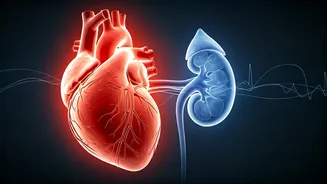
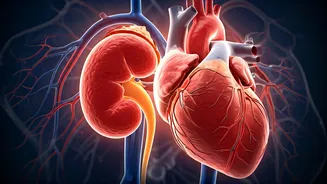
concerning symptoms like swollen ankles, escalating to breathlessness and an eventual diagnosis of early-stage heart failure. Further tests revealed declining kidney function, leading to chronic kidney disease. Rajesh's confusion stemmed from how a well-managed blood sugar level could precipitate such severe cardiac and renal issues. This perplexing situation highlights a critical flaw in how chronic illnesses are often treated: in isolation. For decades, the medical field has compartmentalized the body's systems, assigning each to a specialist. However, modern understanding underscores that organs like the heart, kidneys, and pancreas are not independent entities but are deeply interconnected, engaged in constant communication. When one organ falters, the repercussions are rarely contained, triggering a chain reaction that can affect others. This interconnected system, referred to as the cardio-renal-metabolic axis, is paramount for comprehending chronic diseases, especially in nations like India, where conditions such as diabetes, heart disease, and kidney disorders are concurrently on the rise, making an integrated view of health indispensable.
The Interconnected Axis
The intricate link between diabetes, heart health, and kidney function is rooted in the long-term effects of elevated blood sugar on the body's delicate systems. When glucose levels remain persistently high over years, they inflict damage upon the network of blood vessels throughout the body. The kidneys, which perform the vital function of filtering approximately 180 liters of blood daily, are particularly susceptible to this damage, leading to the gradual development of chronic kidney disease. As the kidneys' filtering capacity diminishes, waste products and excess fluid begin to accumulate in the bloodstream. This buildup consequently increases the workload on the heart, compelling it to pump more forcefully to circulate blood through an increasingly compromised system. Simultaneously, metabolic imbalances inherent in diabetes can trigger hormonal shifts and inflammatory responses that further stress both the cardiovascular and renal systems. Therefore, what might initially appear as disparate medical conditions are, in fact, interconnected manifestations of a systemic breakdown, underscoring the profound impact of diabetes beyond mere glucose regulation. The pancreas also plays a pivotal role within this metabolic framework, regulating blood sugar levels through insulin production. Disruptions in this delicate balance, as seen in Type 2 diabetes, can initiate hormonal and pro-inflammatory cascades that negatively impact the kidneys and cardiovascular system, demonstrating a clear domino effect across multiple organs.
Integrated Care Revolution
Rajesh's journey took a significant turn when he transitioned to an integrated cardiometabolic clinic, a model of healthcare that is progressively gaining traction. This approach shifted from fragmented consultations to a comprehensive evaluation designed to meticulously examine the interplay between his various conditions. Instead of specialists reviewing his results in isolation, they collaborated, pooling their insights to collectively guide treatment decisions. This collaborative approach led to crucial adjustments in his medication, incorporating emerging therapies for diabetes that also offer protective benefits for heart and kidney function. His diet was recalibrated to alleviate strain on all three interconnected systems, and his exercise regimen was tailored to his cardiac tolerance, metabolic control, and renal safety. This marked a fundamental shift from managing three separate diseases to addressing a single, interconnected health challenge. Over an eighteen-month period, Rajesh experienced substantial improvements. His kidney function decline significantly slowed, his breathlessness diminished, and hospital visits became less frequent, allowing him to resume everyday activities with renewed vigor. This integrated model proves that a holistic view, rather than disease-specific treatment, is crucial for optimal patient outcomes.
Prevention and Screening
The critical importance of shifting towards integrated, preventive, and patient-centered healthcare models cannot be overstated. Experts advocate for early screening as cardiometabolic diseases often develop silently for years before any overt symptoms manifest. A combined screening process that assesses blood pressure, blood sugar, and kidney function concurrently can effectively identify risks at an early stage, allowing for timely intervention. Beyond screenings, adopting a proactive lifestyle is paramount in reducing the collective burden on the heart, kidneys, and pancreas. Key preventive measures include balanced nutrition, engaging in regular physical activity, maintaining a healthy weight, and abstaining from smoking. These lifestyle modifications, when implemented consistently, can significantly mitigate the risk of developing or exacerbating these interconnected chronic conditions. The good news is that newer treatments for diabetes are increasingly showing efficacy in addressing the other two conditions as well, offering a more unified approach to management and treatment regimens that consider the impact of medication on all three conditions simultaneously.