The Polypharmacy Puzzle
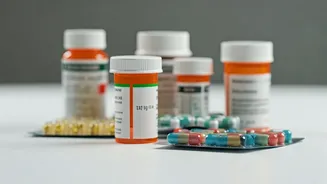
As we age, managing multiple health conditions often leads to taking numerous medications, a situation termed polypharmacy. This is particularly common
among older adults dealing with issues like hypertension, elevated cholesterol, and diabetes, alongside heart conditions such as atrial fibrillation. However, ingesting more than five drugs daily introduces substantial risks, with research indicating that a significant portion of prescriptions for seniors may be unnecessary or even detrimental. Cardiovascular medications, in particular, are frequently flagged as potentially harmful or lacking clear benefits. Experts emphasize the importance of deprescribing, the process of eliminating non-essential medications, to mitigate adverse effects and improve patient well-being. This practice is vital for ensuring that the medications individuals rely on are truly serving their health needs and not inadvertently causing harm or financial strain. The sheer volume of pills can become overwhelming, increasing the likelihood of errors and reducing the quality of life.
Rethinking Blood Pressure Drugs
The landscape of high blood pressure treatment is constantly evolving, with numerous drug classes available. While many medications effectively lower blood pressure, current recommendations are shifting away from beta blockers for long-term management of hypertension. They are no longer the go-to for sustained use post-heart attack and can cause significant dizziness when combined with calcium-channel blockers. Although beta blockers remain valuable for specific patient groups, individuals taking them for high blood pressure might benefit more from alternative drug classes, such as angiotensin-receptor blockers or thiazide diuretics. It's critical to note that abrupt cessation of beta blockers can be dangerous, potentially leading to a rapid heart rate increase and chest pain. Therefore, any adjustments to these medications should be done under strict medical supervision, prioritizing patient safety and optimal therapeutic outcomes.
Heart Attack Prevention Strategies
For many years, low-dose aspirin was a standard recommendation for most middle-aged and older adults to prevent a first heart attack. However, current guidelines have narrowed this recommendation to individuals who have already experienced a heart attack or are at very high risk. For those without existing cardiovascular disease, the potential bleeding risks associated with aspirin often outweigh its preventive benefits. Conversely, the role of statins in preventing heart attacks remains strong. Doctors still recommend that patients continue taking prescribed statins, regardless of age, as recent studies show they effectively reduce cardiovascular disease risks in individuals aged 75 and older without increasing adverse effects. For those on simvastatin, switching to atorvastatin or rosuvastatin may offer enhanced effectiveness and fewer drug interactions. Additionally, niacin is advised against due to its lack of cardiovascular benefits and potential for side effects. Care is also advised with NSAIDs, as prolonged use can elevate the risk of heart attack and stroke.
Diabetes Management Update
Metformin continues to be the cornerstone of treatment for type 2 diabetes, as recommended by major health organizations. While older drug classes like DPP-4 inhibitors, such as sitagliptin and saxagliptin, are rarely prescribed now, more advanced options are available. The current leading add-on therapies for type 2 diabetes are GLP-1 receptor agonists and SGLT2 inhibitors. These modern medications not only help control blood sugar levels but also offer significant cardiovascular protection and contribute to a reduced risk of premature death, making them highly beneficial for long-term patient health and well-being.
Managing Atrial Fibrillation Risks
Individuals diagnosed with atrial fibrillation (afib) typically require anticoagulant medications to minimize stroke risk. Direct oral anticoagulants (DOACs), such as rivaroxaban and apixaban, are generally preferred over warfarin, an older anticoagulant, due to their improved safety and efficacy profiles. Patients currently on warfarin, unless they have a mechanical heart valve, are often advised to consider switching to a DOAC. Furthermore, if a patient taking a DOAC is also on aspirin, it is crucial to consult a doctor about discontinuing the aspirin, as the combination can significantly increase bleeding risk. While DOACs can be more costly, the availability of generic versions is anticipated soon, making them more accessible.
Taking Control of Your Meds
Proactively managing your medications is key to ensuring their continued benefit and safety. The first step is to thoroughly understand the purpose of each drug you are prescribed; if there's any doubt, seek clarification from your doctor. Ideally, your primary care physician should conduct a comprehensive review of all your medications, including over-the-counter drugs and supplements, at least annually. Regularly check your online health portal to verify that the medication list accurately reflects what you are currently taking. Moreover, lifestyle adjustments such as weight loss, dietary improvements, reduced alcohol consumption, and increased physical activity can significantly impact health markers like blood pressure, cholesterol, and blood sugar, potentially allowing for the reduction or elimination of certain medications.