Understanding the Urgency
The familiar tug at a child's ear can quickly escalate into parental concern, disrupting daily life and fostering worry. Ear infections are incredibly
common, with studies indicating that up to 85% of children experience at least one before their third birthday, making it a near-universal experience for parents. While the instinct is to seek immediate medical attention, it's crucial to recognize that not all ear infections necessitate urgent treatment or antibiotics. Many parents understandably feel a sense of urgency due to the child's discomfort and their own anxieties about potential complications. This often leads to over 90% of parents seeking help within 1-2 days of suspecting an infection, driven by a fear of worsening symptoms, hearing loss, or the infection escalating, especially when a child cannot articulate their pain.
Antibiotic Belief vs. Reality
A significant misconception among parents is the belief that antibiotics are always required for ear infections, with over one in three holding this view. This perception heavily influences treatment decisions. However, medical evidence shows that the majority of childhood ear infections resolve spontaneously within a few days. Astonishingly, only about 20% of cases actually benefit from antibiotic treatment. The confusion arises from overlapping symptoms with other illnesses, the immediate pain that feels critical, and the perceived 'quick fix' that antibiotics offer. The widespread overuse of antibiotics, however, contributes to serious issues like diarrhea, allergic reactions, and, more concerningly, the long-term problem of antimicrobial resistance, jeopardizing future treatment efficacy for everyone.
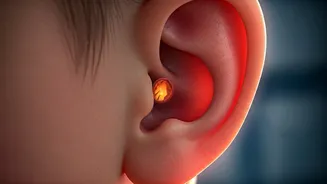
Inside the Infected Ear
Understanding the physiological process behind an ear infection can help alleviate parental anxiety. Typically, an ear infection begins as a consequence of a common cold, leading to fluid accumulation behind the eardrum. This trapped fluid generates pressure and causes discomfort. In many instances, the child's own immune system effectively clears this fluid, resolving the infection naturally. This is the basis for the 'watch and wait' strategy often recommended by healthcare professionals for less severe cases. Supportive care like pain management, adequate rest, and hydration are usually sufficient. Yet, this waiting period can feel interminable for parents, particularly when interrupted sleep and persistent discomfort plague their child.
Life's Disruptions Influence Decisions
The decision to consult a doctor about a child's ear infection isn't solely dictated by the severity of symptoms; real-life circumstances play a significant role. Research indicates that factors like parental absence from work, disruptions to childcare arrangements, and visible signs such as ear discharge can significantly increase the perceived urgency. Essentially, the impact of the illness on the family's daily routine often dictates the speed at which medical help is sought. This explains why many families opt for immediate solutions, even when the condition might naturally improve without medical intervention. Recognizing these external pressures helps to understand the parental drive for swift action.
When to Wait or Seek Care
Navigating the decision-making process for ear infections can be simplified with clear guidelines. Parents can generally adopt a 'wait and monitor' approach if their child is experiencing mild ear pain, has a low-grade or no fever, and symptoms have only recently appeared. Conversely, immediate medical attention is warranted if the pain is severe or intensifying, the fever is high (above 39°C or 102.2°F), there is any fluid discharge from the ear, or if the child is very young, specifically under six months old. Consulting a pharmacist or doctor can provide further guidance, but asking whether immediate treatment or careful observation is needed is a critical first step, often revealing that the situation is less urgent than it initially appears.
Effective Home Care Strategies
Home-based care significantly contributes to a child's recovery from ear infections, often more than parents realize. Simple, consistent actions can effectively alleviate discomfort and support the healing process. These include administering age-appropriate pain relievers, as recommended by a healthcare provider, ensuring the child remains well-hydrated, and encouraging ample rest beyond their usual routine. Keeping the child in an upright position can also help reduce pressure within the ear canal. Beyond physical care, parental reassurance is invaluable. A calm and supportive demeanor from a parent can greatly enhance a child's sense of security, even amidst pain and discomfort, contributing to a more positive recovery experience.
Building Confidence and Clarity
A notable gap exists in the communication between healthcare providers and parents regarding antibiotic use for ear infections. Studies reveal that only 28% of parents report receiving clear guidance on this matter, despite 43% expecting it. This lack of clear advice breeds confusion, often leading to unnecessary prescriptions. Public health experts emphasize the critical need for enhanced awareness campaigns led by healthcare professionals, including pharmacists and doctors. By better educating parents on when antibiotics are truly beneficial versus when they are not, a foundation for more informed and calmer decision-making can be built. This ultimately leads to more effective outcomes for children and contributes to tackling the broader issue of antibiotic resistance.
Beyond the Medical Issue
An ear infection in a child is rarely confined to a purely medical diagnosis; it encompasses emotional strain, routine disruption, and tests of parental patience. However, these challenges also present invaluable opportunities to build parental confidence in managing common childhood health concerns. By understanding the nuances of when to intervene medically and when to patiently observe, parents can navigate these situations with greater assurance. This informed approach not only leads to better management of the immediate illness but also fosters a sense of empowerment for future health challenges, demonstrating that effective care often lies in a balanced approach between action and watchful waiting.