Genetic Roots of Celiac
Celiac disease is a health condition where an individual's genetic makeup is a significant factor in its development. This autoimmune disorder is triggered
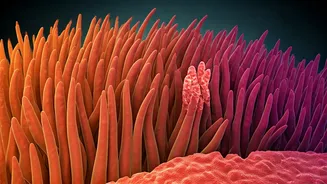
by the ingestion of gluten, a protein found in grains like wheat, barley, and rye. When consumed by individuals with Celiac disease, gluten prompts an exaggerated immune response. This overactive immune system mistakenly targets and damages the lining of the small intestine, specifically the villi. These villi are vital finger-like projections responsible for absorbing nutrients from food. The damage to the villi impairs nutrient absorption, leading to various health issues. While Celiac disease is considered rare, affecting approximately 1 in 100 people globally, a striking statistic reveals that only about 30% of affected individuals receive a proper diagnosis. This highlights a significant gap in awareness and identification of the condition. The hereditary component is substantial; individuals with a first-degree relative diagnosed with Celiac disease face a tenfold increased risk of developing the condition themselves, underscoring the importance of family history in assessing susceptibility.
Gluten's Impact on Intestine
The consumption of gluten is the primary trigger for the cascade of events in Celiac disease. For those afflicted, gluten is not merely a food component but an instigator of an aggressive autoimmune reaction. This reaction disproportionately impacts the small intestine, the primary site for nutrient absorption. The immune system's overzealous response directs its attack towards the villi, the delicate, hair-like structures lining the small intestine. Normally, these villi possess a vast surface area, facilitating efficient absorption of essential vitamins, minerals, and macronutrients. However, in Celiac disease, the immune attack flattens these villi, severely compromising their ability to function. This damage results in malabsorption, where the body cannot adequately extract the nutrients it needs from food. Consequently, individuals may suffer from deficiencies in vital nutrients, leading to a range of symptoms. It's crucial to differentiate this from gluten sensitivity or intolerance, where individuals may experience digestive distress upon consuming gluten, but their small intestines do not undergo the same kind of structural damage and malabsorption characteristic of Celiac disease.
Celiac vs. Gluten Intolerance
Distinguishing Celiac disease from gluten intolerance is paramount for appropriate management and understanding of health implications. While both conditions involve adverse reactions to gluten, the underlying mechanisms and physiological consequences differ significantly. Celiac disease is a specific autoimmune disorder where the immune system's response to gluten directly harms the small intestine's villi. This damage impairs nutrient absorption, potentially leading to malnutrition and a host of related health problems, including anemia, osteoporosis, and neurological issues. The genetic predisposition is a strong indicator for Celiac disease. Conversely, gluten intolerance, also known as non-celiac gluten sensitivity, presents with symptoms that can mimic Celiac disease, such as bloating, abdominal pain, and fatigue, after consuming gluten. However, individuals with gluten intolerance do not exhibit the autoimmune damage to the small intestine or the specific antibodies associated with Celiac disease. Their digestive system may react to gluten, but the structural integrity and absorptive function of the villi remain intact. Accurately diagnosing Celiac disease is critical as it requires strict lifelong adherence to a gluten-free diet to prevent long-term health complications.