Understanding HPV's Role
The vast majority of cervical cancer cases are inextricably linked to persistent infections with high-risk strains of the Human Papillomavirus (HPV). Dr.
Sathyanarayanan highlights that squamous cell carcinoma of the cervix is almost exclusively caused by HPV. While HPV is common and most infections resolve on their own, the concern arises when specific high-risk types linger in the body for extended periods. These persistent infections can subtly alter cervical cells over time, paving the way for cancer development. This underscores the critical importance of understanding HPV as the primary driver of the disease and focusing prevention efforts on mitigating its transmission and impact.
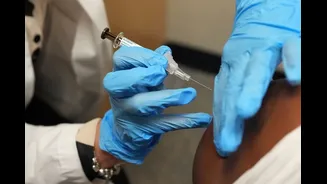
The Power of HPV Vaccination
A cornerstone of cervical cancer prevention lies in the HPV vaccine, which effectively neutralizes the most dangerous HPV strains. For optimal protection, the vaccine is most impactful when administered before any exposure to the virus, ideally between the ages of 9 and 14. However, its benefits extend to individuals up to 26 years old, and in some instances, even beyond with professional medical guidance. Nations that have embraced widespread HPV vaccination programs have already witnessed a dramatic reduction in pre-cancerous cervical lesions and full-blown cervical cancers. India's inclusion of HPV vaccination in its National Immunization Programme signifies a crucial step forward, framing this intervention not as a lifestyle choice, but as a fundamental cancer prevention strategy vital for public health.
Smoking's Detrimental Impact
Beyond its well-known effects on the lungs, smoking significantly compromises the body's defenses against HPV. As explained by medical experts, tobacco use weakens the immune system, making it considerably more challenging for the body to naturally clear HPV infections. Shockingly, harmful chemicals from tobacco smoke have been detected within cervical mucus, directly impacting the cervix. When the immune system is compromised, HPV infections are more likely to persist for longer durations. This prolonged presence of the virus escalates the risk of developing cervical cancer. Fortunately, women who make the decision to quit smoking can gradually rebuild their immune strength. While the elevated risk doesn't vanish immediately, it steadily diminishes over time, demonstrating that prioritizing whole-body health is integral to cervical cancer prevention.
Early Detection Through Screening
Cervical cancer often begins its insidious progression without any discernible symptoms, making early detection through regular screening absolutely crucial. Precancerous cellular changes rarely manifest as pain, bleeding, or other obvious signs. Screening methods, such as Pap smears, HPV DNA testing, and visual inspection techniques (especially in resource-limited settings), are designed to identify these cellular abnormalities before they transform into cancer. Despite ongoing national screening programs in India, coverage remains inconsistent, particularly in rural areas. Therefore, it is imperative for women aged 30 to 65 to undergo periodic screening as recommended by their gynecologists. Viewing screening as a proactive health strategy, rather than a reaction to symptoms, is key to silent risk mitigation.
Safe Practices and Awareness
The primary mode of HPV transmission is through sexual contact. Employing safe sexual practices, such as consistent condom use, can significantly reduce the likelihood of HPV transmission, although it doesn't offer complete elimination of risk. Limiting the number of sexual partners and delaying the onset of sexual activity are also effective strategies for lowering exposure to high-risk HPV strains. In India, open discussions about sexual health can still be challenging, but avoiding these conversations does not curtail infection; it only hinders prevention efforts. Public health is profoundly advanced when open awareness replaces stigma and silence, empowering individuals to take informed decisions about their well-being and reducing the burden of diseases like cervical cancer.
Holistic Prevention and Support
Preventing cervical cancer is a collective endeavor that extends beyond individual responsibility, requiring robust support from families, healthcare providers, educators, and policymakers. The scientific foundation for prevention is firmly established: vaccines are effective, screening works, and early treatment yields excellent outcomes. Challenges often arise from gaps in access, insufficient awareness, and a lack of prioritization. The distressing reality is that one woman dies every 8 minutes in India from cervical cancer, a statistic that underscores the urgency of these prevention strategies. This preventable tragedy often stems from delayed diagnoses, missed screenings, or a failure to vaccinate. Recognizing that cervical cancer develops slowly over years presents a critical window for detection and prevention, emphasizing that no woman should face a cancer diagnosis due to a lack of timely information or resources.