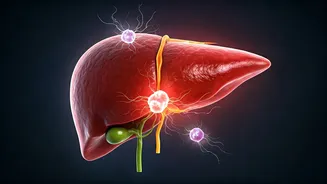
Ammonia's Hidden Role
Our bodies process protein, generating ammonia, a substance normally converted into urea by the liver and excreted. However, when the liver is compromised
by conditions like cirrhosis, fatty liver disease, or chronic hepatitis, this crucial detoxification process can falter. This leads to an accumulation of ammonia in both the liver tissue and bloodstream. Intriguingly, scientific investigations, notably by Rutgers University and published in Science Advances, have revealed that liver tumors may exploit this excess ammonia. Cancer cells appear to repurpose this waste product, using it as a building block for amino acids and nucleotides. These components are vital for rapid cell division and DNA replication, essentially providing fuel for the malignancy to thrive. This suggests that ammonia overload isn't just a consequence of liver damage but can actively promote cancer progression.
Dietary Protein and Tumor Growth
In a compelling study led by Wei-Xing Zong, researchers investigated the impact of dietary protein levels on liver tumor development in mice. By reducing the protein intake of mice prone to developing tumors, the study aimed to decrease the production of ammonia. The results were significant: tumor growth was noticeably slower, and the mice demonstrated extended lifespans across various liver cancer models. This effect was further underscored when the researchers genetically impaired the liver's ammonia-clearing urea cycle. In these instances, ammonia levels surged, leading to accelerated tumor growth and a decline in survival rates. These findings strongly indicate that excessive ammonia, driven by protein metabolism, plays a central role in driving liver cancer, rather than being a mere side effect of genetic mutations.
Tumor Environment Shifts
Beyond merely slowing tumor growth, the low-protein diet induced other beneficial changes within the cancerous growths. The study observed a reduction in cellular proliferation, meaning cancer cells divided less frequently. Furthermore, the signaling pathways associated with fibrosis—the scarring of liver tissue—were dialed down. Key growth pathways within the tumors also showed reduced activity. Essentially, the cancer cells on the restricted protein regimen found it more challenging to acquire the nitrogen necessary for their rapid multiplication. This suggests that lowering protein intake not only limits the fuel source but also fundamentally alters the internal environment of the tumor, making it less conducive to aggressive expansion and survival.
Cautious Outlook for Humans
It is crucial to emphasize that these findings, while promising, are not a green light for widespread protein restriction in cancer patients. Many individuals undergoing cancer treatment require adequate protein to maintain muscle mass, strength, and to support the body's recovery processes. Insufficient protein intake can lead to detrimental effects such as weakness and malnutrition, particularly in those who are already frail. The observed benefits of reduced protein seem to be contingent on the liver's impaired ability to handle normal ammonia loads. Therefore, this dietary strategy is not universally applicable and requires careful consideration of individual health status and treatment protocols. More research is needed to determine its specific applicability.
Future Avenues and Research
For individuals managing pre-existing liver conditions, such as those stemming from alcohol abuse, viral hepatitis, or non-alcoholic fatty liver disease (NAFLD), this research opens up an intriguing question: could a carefully controlled, lower protein diet be a component of managing their cancer risk or slowing disease progression? The researchers themselves urge caution, stressing that results from animal studies do not automatically translate to humans. Rigorous clinical trials are essential to establish safe protein intake levels, identify patient groups most likely to benefit, and ensure that such dietary interventions do not cause unintended harm. This ongoing exploration highlights the complex interplay between metabolism and cancer, suggesting that future therapeutic strategies might target ammonia and nitrogen metabolism, potentially offering a new approach for at-risk populations.