The Misconception of Diabetes
A prevalent, yet dangerous, misconception in healthcare, particularly in India, is that Type 2 diabetes exclusively targets individuals who are overweight.
This assumption frequently leads to delayed diagnoses, as evidenced by numerous patients presenting with significantly elevated HbA1c levels (like 8.2%) despite maintaining a healthy weight, often with a BMI of 22 or below. These individuals may have been previously reassured by medical professionals that they couldn't possibly have diabetes because they didn't 'look the part.' Consequently, precious months, or even years, of the critical early intervention window are lost before they seek more thorough evaluation, by which point substantial metabolic damage may have already occurred. This delayed diagnosis is a major concern, especially given India's high global prevalence of lean diabetes.
Thin Outside, Fat Inside
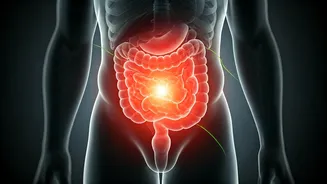
The standard Body Mass Index (BMI) is a notoriously inaccurate measure of metabolic health for the Indian population, as it was originally developed using European demographics and solely assesses total body weight relative to height, neglecting crucial body composition. Consequently, an Indian individual with a seemingly healthy BMI of 23 might still harbor dangerous accumulations of visceral fat – the type of fat that surrounds vital internal organs like the liver, pancreas, and intestines – while appearing outwardly slender. To address this, experts advocate for utilizing the waist-to-height ratio as a more reliable indicator, flagging a ratio above 0.5 as a significant warning sign, irrespective of what the weighing scale suggests. This metabolically active visceral fat contributes directly to insulin resistance by releasing free fatty acids into the bloodstream and promoting chronic, low-grade inflammation throughout the body.
Why Standard Tests Fail
Routine diabetes screening protocols often fall short in identifying early metabolic disturbances in individuals who appear lean. The conventional annual fasting glucose test, for instance, is largely ineffective for early detection; by the time fasting glucose levels deviate from the norm, metabolic damage has typically been developing for years. More sensitive tests are therefore recommended to measure insulin resistance more directly. Elevated fasting insulin levels, specifically above 10 µIU/mL in a lean individual, or a high HOMA-IR score, should prompt further investigation rather than providing reassurance. For some patients who present as metabolically healthy based on standard laboratory results, continuous glucose monitoring (CGM) can reveal alarming post-meal glucose spikes, with levels reaching 180–200 mg/dL after eating, even when fasting numbers appear normal, highlighting the limitations of standard tests.
The Indian Diet Connection
Dietary habits play a significant role in the escalating rates of lean diabetes within India. A typical Indian vegetarian diet, often characterized by a high intake of rice, roti, and dal, coupled with insufficient protein, is essentially a high-carbohydrate meal plan. For individuals genetically predisposed to insulin resistance, this macronutrient imbalance can exacerbate metabolic dysfunction. The core issue isn't necessarily overeating but consuming an imbalanced mix of nutrients. By restructuring diets to significantly increase protein intake to 25–30 grams per meal, reducing refined carbohydrates, and incorporating healthy fats like ghee or olive oil, improvements in metabolic markers can be observed within weeks, often without substantial changes in body weight.
Redefining Metabolic Health
Lean diabetes is not an inexplicable medical phenomenon but rather a consequence of inadequate screening methodologies. The reliance on BMI as the primary gauge for metabolic health needs to be reassessed. Instead, greater emphasis should be placed on metrics that truly reflect metabolic status, such as visceral fat levels, fasting insulin concentrations, and waist circumference. In India, an outwardly slim physique does not guarantee metabolic well-being. The body visible in the mirror might not be the source of illness; it's frequently the concealed, internal fat that poses the most significant health risks, underscoring the need for a more nuanced approach to diabetes detection and management.