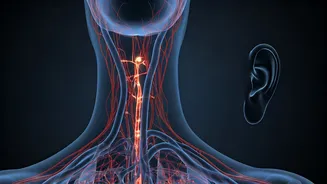
Stroke Risks Magnified
Untreated high blood pressure stands as the primary culprit behind strokes, a leading cause of mortality. Individuals with readings of 160/95 mm Hg or higher
face approximately a fourfold increased risk of stroke compared to those with normal blood pressure. This condition can manifest as an ischemic stroke, caused by a blocked artery supplying the brain, or a hemorrhagic stroke, resulting from a ruptured blood vessel near or within the brain. The persistent force of elevated blood pressure weakens arterial walls, making them prone to blockages and ruptures, thereby significantly elevating the likelihood of these life-threatening cerebrovascular events.
Cardiovascular System Under Siege
Hypertension significantly compromises the integrity of your blood vessel walls, rendering them more vulnerable to atherosclerosis, a dangerous accumulation of fatty deposits. When these plaques form within the coronary arteries that nourish the heart muscle, it results in coronary artery disease. Heart attacks occur when these arteries become completely obstructed, either by a blood clot forming on a ruptured plaque or by debris such as cholesterol and dead cells. Furthermore, fragments of these plaque deposits, termed emboli, can detach from major arteries like the aorta, travel through the bloodstream, and obstruct vessels elsewhere, leading to circulatory issues in the legs or precipitating strokes by blocking arteries supplying the brain. The presence of high cholesterol alongside high blood pressure amplifies these risks, accelerating the development of serious cardiovascular complications.
Heart Muscle Strain
The relentless pressure of high blood pressure compels the heart to exert considerably more effort to circulate blood throughout the body. Consequently, the left ventricle, the heart's primary pumping chamber, undergoes thickening and muscle enlargement to generate stronger contractions. While this adaptive response, known as left ventricular hypertrophy, initially aims to overcome the increased resistance, it eventually becomes detrimental. As the heart muscle grows, its demand for oxygen escalates, but the coronary arteries, themselves thickened and narrowed by hypertension, struggle to deliver adequate oxygen. This oxygen deficit can trigger angina, or chest pain, and in severe cases, can culminate in a heart attack.
Heart Failure Development
The combined strain of left ventricular hypertrophy and compromised coronary arteries, both exacerbated by persistent high blood pressure, can ultimately lead to heart failure. This condition, also referred to as congestive heart failure, signifies the heart's diminished capacity to pump blood effectively throughout the body. Individuals with uncontrolled hypertension are twice as likely to develop heart failure compared to those with normal blood pressure. Symptoms may include profound fatigue and weakness due to insufficient blood supply to muscles, breathlessness, and fluid accumulation (edema) in the lungs, feet, ankles, and legs, indicating the body's struggle to manage fluid balance.
Irregular Heart Rhythms
Prolonged, uncontrolled high blood pressure is identified as the most prevalent antecedent to atrial fibrillation, a disordered heart rhythm that typically emerges after the age of 65. Sufferers of atrial fibrillation experience intermittent episodes where the upper chambers of their heart quiver erratically. This chaotic movement causes blood to stagnate and pool within these chambers, fostering the formation of clots. If these clots dislodge and travel to the brain, they can trigger a stroke, increasing the risk of stroke by approximately fivefold.
Cognitive Decline
High blood pressure can significantly accelerate the process of atherosclerosis, thereby contributing to the onset of dementia, a condition characterized by a decline in memory and thinking abilities that impairs daily functioning. Impaired circulation resulting from atherosclerosis can lead to the formation of dead tissue areas within the brain due to insufficient blood supply to medium and large arteries. Additionally, high blood pressure can directly damage the brain's smaller arteries. When blood flow in one of these smaller vessels significantly slows or ceases, it can result in a minor stroke, often termed a 'silent' stroke due to its lack of immediate symptoms. These strokes may occur in multiple brain regions, but their small localized impact means symptoms might not be apparent until a substantial amount of brain tissue has been damaged. This phenomenon, known as vascular dementia, is a recognized contributor to memory loss in older adults.
Kidney Function Impairment
Your kidneys, responsible for filtering waste from your blood, play a critical role in regulating blood pressure by managing water and sodium levels. Elevated blood pressure prompts the kidneys to excrete excess water and sodium, helping to lower pressure by reducing circulating blood volume through urination. Conversely, low blood pressure signals the kidneys to retain these substances to boost blood volume. However, individuals with hypertension often retain too much water and sodium. Uncontrolled high blood pressure is the second leading cause of kidney failure, accounting for roughly 25% of new cases, underscoring its detrimental impact on renal health.
Vision and Eye Health
High blood pressure poses a serious threat to vision by damaging the delicate blood vessels within the eye. These arteries, crucial for supplying oxygen and nutrients to the retina, can narrow or rupture, leading to bleeding into the retina itself. The resultant fluid accumulation can distort vision and create scars that impair sight permanently. Swelling of the optic nerve, which transmits visual information to the brain, can also occur, potentially causing vision loss. Persistent, unmanaged hypertension can ultimately lead to blindness, emphasizing the importance of regular eye examinations alongside blood pressure management.