What's Happening?
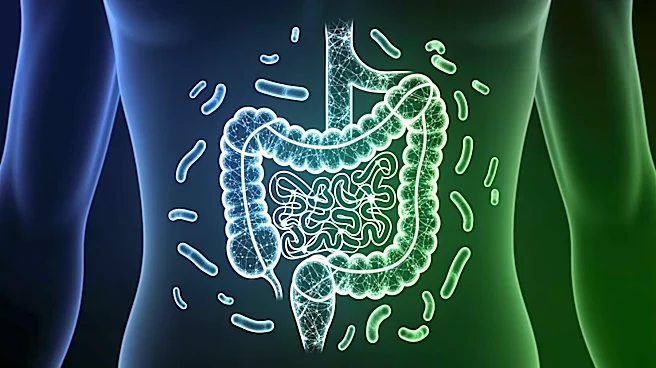
Researchers at Case Western Reserve University have discovered a significant link between gut bacteria and the progression of Amyotrophic Lateral Sclerosis (ALS) and Frontotemporal Dementia (FTD). The study, published in Cell Reports, reveals that certain
bacterial sugars in the gut can trigger immune responses that lead to brain cell damage. This discovery sheds light on why some individuals with genetic predispositions develop these diseases while others do not. The research team, led by Aaron Burberry and Alex Rodriguez-Palacios, found that harmful forms of glycogen produced by gut bacteria are present in 70% of ALS/FTD patients studied, compared to only one-third of individuals without these conditions. The findings suggest that these bacterial sugars could serve as new targets for treatment, potentially leading to therapies that focus on the gut-brain connection.
Why It's Important?
This discovery is crucial as it opens new avenues for treating ALS and FTD, two debilitating neurological disorders with limited treatment options. By identifying gut bacteria as a potential trigger for these diseases, researchers can develop targeted therapies that may slow or prevent disease progression. This is particularly significant for individuals with the C90RF72 mutation, the most common genetic cause of ALS and FTD, as it provides insight into why not all carriers develop the disease. The study also highlights the potential for using gut bacteria as biomarkers to identify patients who might benefit from specific treatments, offering hope for improved patient outcomes.
What's Next?
The research team plans to conduct larger studies to further explore the role of gut bacteria in ALS and FTD. They aim to survey gut microbiome communities in patients before and after disease onset to better understand when and why harmful glycogen is produced. Additionally, clinical trials are being considered to test whether reducing these bacterial sugars can slow disease progression. These trials could begin within a year, potentially leading to new treatment strategies that focus on the gut-brain axis.